Details
The research, published in JAMA Network Open, compared Optum patients in fully accountable Medicare Advantage plans — where Optum care teams take full financial and clinical responsibility for patients — with a national random sample of administrative claims data for patients served by traditional Medicare fee-for-service.
In every metric examined, the health of patients who were in Optum’s fully accountable care model showed statistically significant improvements.
By the numbers
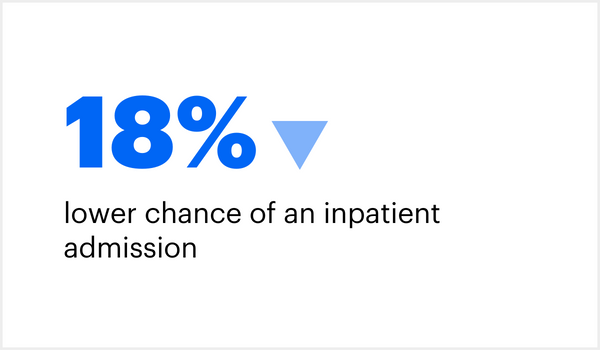
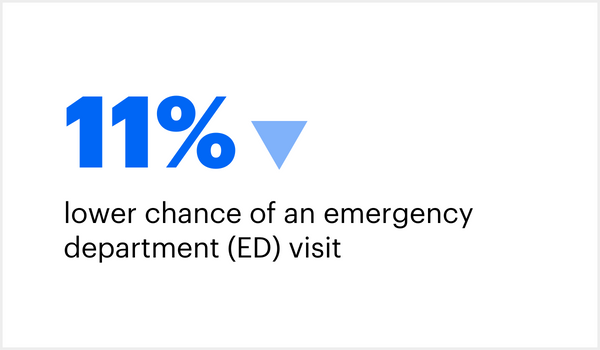
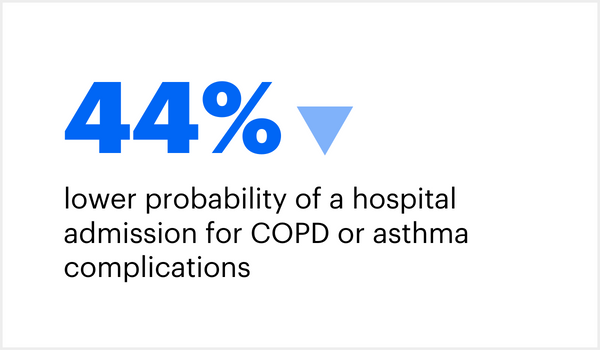
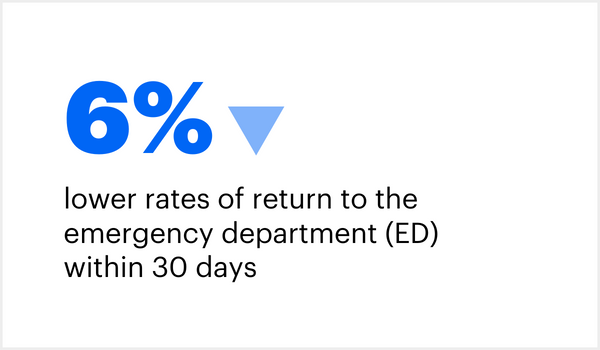
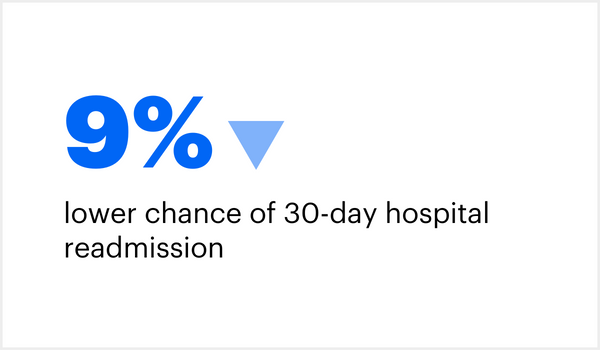
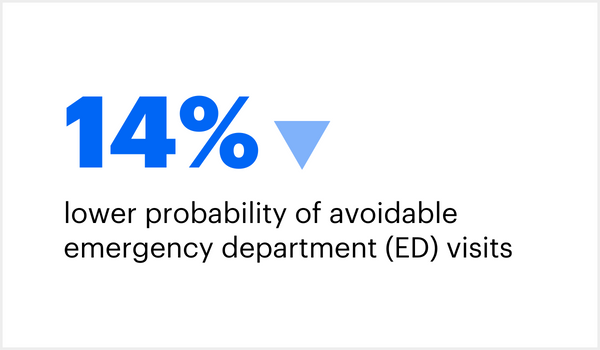
When compared to Medicare fee-for-service patients, those in fully accountable care plans had:
Patient service and beyond
This research demonstrates how Optum and UnitedHealthcare’s unique approach to value-based care better serves Medicare Advantage patients and helps to deliver better health outcomes. The study also contributes to the body of evidence showing how Medicare Advantage — with consumer-focused plans and additional benefits not available in FFS — helps people find the best path of care at the right place and time, while reducing costs through modernized and coordinated clinical programs that address their unique needs.




Share This Story