Newsroom
The UnitedHealth Group newsroom provides timely updates, expert insights and comprehensive coverage on health care advancements, policy changes and company initiatives.
Press Releases
UNITEDHEALTH GROUP ANNOUNCES EARNINGS RELEASE DATE
UnitedHealthcare’s AI-powered Capability Helps Identify and Distribute More Cash Payments for Members
UnitedHealthcare to Support Rural Hospitals with Accelerated Medicare Advantage Payments, Providing Immediate Cash-Flow Relief
UNITEDHEALTH GROUP ANNOUNCES EARNINGS RELEASE DATE
UnitedHealth Group Reports Third Quarter 2025 Results and Raises Full Year 2025 Earnings Outlook
UnitedHealthcare’s 2026 Medicare Advantage Plans Deliver Value, Access and Consumer Choice
UnitedHealth Group Announces Earnings Release Date
UnitedHealth Group Announces Changes to Leadership Team
UnitedHealth Group Re-Establishes Full Year Outlook and Reports Second Quarter 2025 Results
EARNINGS TELECONFERENCE MOVES TO EARLIER TIME ON JULY 29
UnitedHealth Group Recommends Shareholders Reject "Mini-Tender" Offer by Tutanota
UnitedHealth Group today announced that it recently became aware of an unsolicited “mini-tender” offer by Tutanota LLC (Tutanota) to purchase up to 175,000 shares of UnitedHealth Group’s common stock, representing significantly less than 1% of UnitedHealth Group’s common stock outstanding.
UnitedHealth Group Updates on Annual Shareholder Meeting, Board Actions
UnitedHealth Group provided updates on its 2025 annual shareholder meeting and actions taken by its Board of Directors.
UNITEDHEALTH GROUP ANNOUNCES EARNINGS RELEASE DATE
UnitedHealth Group Announces Leadership Transition
UnitedHealth Group Reports First Quarter 2025 Results and Revises Full Year Guidance
UnitedHealth Group reported first quarter 2025 results and revised its outlook for the year.
UNITEDHEALTH GROUP ANNOUNCES EARNINGS RELEASE DATE
UnitedHealth Group will release its first quarter 2025 financial results on Thursday, April 17, 2025, before the market opens, and will host a teleconference at 8:45 a.m. ET to discuss the results with analysts and investors.
Optum Rx to Modernize Pharmacy Payment Models
Effective immediately and with full implementation by January 2028, Optum Rx will align payment models more closely to the costs pharmacies may face due to manufacturer pricing actions.
Optum Rx Further Simplifies Consumer Access to Prescription Drugs
Optum Rx is committed to making prescription drugs more affordable and the pharmacy experience simpler for consumers with chronic conditions, eliminating up to 25% of reauthorizations, which is equal to more than 10% of overall pharmacy prior authorizations.
UnitedHealth Group Reports 2024 Results
UnitedHealth Group (NYSE: UNH) reported full year and fourth quarter 2024 results reflecting diversified growth in serving people more extensively at Optum and UnitedHealthcare.
UNITEDHEALTH GROUP ANNOUNCES EARNINGS RELEASE DATE
UnitedHealth Group will release its fourth quarter and full year 2024 financial results on Thursday, January 16, 2025, before the market opens, and will host a teleconference at 8:45 a.m. ET to discuss the results with analysts and investors.
UnitedHealth Group Updates Business Outlook Ahead of Investor Conference
UnitedHealth Group issued financial guidance ahead of its annual Investor Conference which takes place on December 4, beginning at 8:00 a.m. ET.
UnitedHealth Group to Host 2024 Investor Conference
UnitedHealth Group will host its annual Investor Conference for analysts and institutional investors in New York City on Wednesday, December 4, 2024, beginning at 8:00 a.m. EST.
UnitedHealth Group Board Authorizes Payment of Quarterly Dividend
The UnitedHealth Group board of directors has authorized payment of a cash dividend of $2.10 per share, to be paid on December 17, 2024, to all shareholders of record of UNH common stock as of the close of business December 9, 2024.
UnitedHealthcare Expands Its Individual & Family Plans on the Health Insurance Marketplace to 30 States
UnitedHealthcare has announced a significant expansion of its Individual & Family Affordable Care Act Marketplace plans, now offering coverage in 30 states.
UnitedHealth Group Reports Third Quarter Results
UnitedHealth Group (NYSE: UNH) reported third quarter 2024 results reflecting broad-based growth in the number of people served by Optum and UnitedHealthcare.
UnitedHealthcare Commits $335,000 to Idaho Organizations To Expand Health Care Workforce and Access To Care
UnitedHealthcare today announced a $335,000 commitment in funding to Idaho organizations to help close gaps in care among underserved communities, including people in rural areas, individuals with chronic conditions and seniors.
UnitedHealthcare 2025 Medicare Advantage Plans Deliver Choice, Stability
UnitedHealthcare today introduced its 2025 Medicare Advantage plans, featuring more choice, broad access to care and stability in the most popular benefits to meet the evolving and varied needs of Medicare consumers.
UnitedHealthcare Community Plan of Kansas Awarded NCQA Health Equity Accreditation
UnitedHealthcare Community Plan of Kansas has been awarded Health Equity Accreditation by the National Committee for Quality Assurance.
UnitedHealthcare Community Plan of New Mexico invests $250,000 to provide integrated health care services to K-12 students
UnitedHealthcare Community Plan of New Mexico today announced a $250,000 investment in school-based health care provider Goodside Health to expand access to integrated physical and behavioral health care services to 50 New Mexico schools.
UNITEDHEALTH GROUP ANNOUNCES EARNINGS RELEASE DATE
UnitedHealth Group will release its third quarter 2024 financial results on Tuesday, October 15, 2024, before the market opens, and will host a teleconference at 8:45 a.m. ET to discuss the results with analysts and investors.
UnitedHealthcare Awards $114,500 to Seven Organizations to Address Social Drivers of Health in Iowa
UnitedHealthcare has awarded $114,500 to seven organizations aimed at improving health outcomes across Iowa.
UnitedHealth Group and Goodwill® Partner to Expand Career Pathways Training to Foster Healthier Communities
UnitedHealth Group and Goodwill Industries International today announced a three-year, $4.5 million strategic partnership to increase access to education and training, health-related social needs support and workforce development opportunities in 25 states through 38 Goodwill® organizations.
UnitedHealthcare Community Plan of North Carolina Awarded NCQA Health Equity Accreditation
UnitedHealthcare Community Plan of North Carolina announced it has been awarded Health Equity Accreditation by the National Committee for Quality Assurance.
UnitedHealthcare Selected by the Florida Agency for Health Care Administration to Continue Serving Florida Medicaid Members
UnitedHealthcare Community Plan of Florida has been selected to serve Medicaid members in three regions in collaboration with the Florida Agency for Health Care Administration.
UnitedHealth Group’s Response to the Wall Street Journal
Setting the record straight on HouseCalls, Medicare Advantage and the demonstrably superior health outcomes and cost savings delivered to more than 33 million American seniors each year.
UnitedHealth Group Board Authorizes Payment of Quarterly Dividend
The UnitedHealth Group board of directors has authorized payment of a cash dividend of $2.10 per share, to be paid on September 24, 2024, to all shareholders of record of UNH common stock as of the close of business September 16, 2024.
UnitedHealthcare Selected by the State of Rhode Island to Continue Serving Medicaid Members
UnitedHealthcare Community Plan of Rhode Island has been selected by the State of Rhode Island to serve Medicaid members through the Medicaid Managed Care Services program.
UnitedHealth Group Reports Second Quarter Results
UnitedHealth Group (NYSE: UNH) reported second quarter 2024 results reflecting broad-based growth at Optum and UnitedHealthcare.
UNITEDHEALTH GROUP ANNOUNCES EARNINGS RELEASE DATE
UnitedHealth Group will release its second quarter 2024 financial results on Tuesday, July 16, 2024, before the market opens, and will host a teleconference at 8:45 a.m. ET to discuss the results with analysts and investors.
UnitedHealthcare Invests $1 Million to Provide Integrated Health Care Services to K-12 Students in Texas
UnitedHealthcare Community Plan of Texas has announced a $1 million investment in school-based health care provider Goodside Health to conduct EPSDT (Early and Periodic Screening, Diagnosis and Treatment) wellness events in 200 schools located throughout Texas.
UnitedHealth Group Provides Updates on Annual Shareholder Meeting, Board Actions
UnitedHealth Group provided updates on its 2024 annual shareholder meeting and actions by its Board of Directors.
UnitedHealthcare Invests $1.5 Million to Expand School-Based Health Care Services Across Iowa
UnitedHealthcare Community & State of Iowa has announced a $1.5 million investment in school-based telehealth to expand access to mental health care for K-12 students in Iowa.
State of Kansas Selects UnitedHealthcare to Serve Medicaid and Children’s Health Insurance Program Beneficiaries
UnitedHealthcare Community Plan of Kansas has been selected by the State of Kansas as one of three managed care organizations to administer KanCare, the statewide Medicaid and Children’s Health Insurance Program, effective Jan. 1, 2025.
The Arc and United Health Foundation Launch $2.5M Partnership to Tackle Mental Health Crisis for People with Disabilities
The United Health Foundation, the philanthropic foundation of UnitedHealth Group (NYSE: UNH), has awarded The Arc of the United States a three-year, $2.5 million grant to improve mental health care for people with intellectual and developmental disabilities (IDD).
United Health Foundation Announces $2 Million Grant to Native American Connections to Establish Mobile Health Initiative
The United Health Foundation, the philanthropic foundation of UnitedHealth Group (NYSE: UNH), today announced a three-year, $2 million grant partnership with Native American Connections (NAC).
UnitedHealth Group Updates on Change Healthcare Cyberattack
UnitedHealth Group (NYSE: UNH) is announcing support for people who may be concerned about their personal data potentially being impacted based on preliminary findings from the ongoing investigation and review of the data involved in the malicious criminal cyberattack on Change Healthcare.
UnitedHealthcare Selected to Serve Medicaid Members in Michigan Through the Comprehensive Health Care Program
The Michigan Department of Health and Human Services (MDHHS) has selected UnitedHealthcare Community Plan of Michigan as one of the nine managed care organizations to administer the Comprehensive Health Care Program (CHCP).
UnitedHealth Group Reports First Quarter Results
UnitedHealth Group (NYSE: UNH) reported first quarter 2024 results reflecting broad-based growth at Optum and UnitedHealthcare, medical care activity consistent with expectations and the impact of the recent cyberattack on Change Healthcare.
UnitedHealthcare Provides $180,000 Investment to United Disabilities Services Foundation to Support Aging and Disability Services in Pennsylvania
UnitedHealthcare Community Plan of Pennsylvania has provided a $180,000 investment to the United Disabilities Services Foundation (UDSF) to support aging and disability services for adults across the state.
UNITEDHEALTH GROUP ANNOUNCES EARNINGS RELEASE DATE
UnitedHealth Group will release its first quarter 2024 financial results on Tuesday, April 16, 2024, before the market opens, and will host a teleconference at 8:45 a.m.
UnitedHealth Group Cyberattack Status Update
UnitedHealth Group (NYSE: UNH) continues to make progress in mitigating the impact to consumers and care providers of the unprecedented cyberattack on the U.S. health system and the Change Healthcare services, while continuing to expand financial assistance to affected providers.
UnitedHealth Group Update on Change Healthcare Cyberattack
UnitedHealth Group continues to make substantial progress in mitigating the impact to consumers and care providers of the unprecedented cyberattack on the U.S. health system and the Change Healthcare claims and payment infrastructure.
UnitedHealth Group Board Authorizes Payment of Quarterly Dividend
The UnitedHealth Group (NYSE: UNH) board of directors has authorized payment of a cash dividend of $1.88 per share, to be paid on March 19, 2024, to all shareholders of record of UNH common stock as of the close of business March 11, 2024.
UnitedHealthcare of California Awarded National Committee for Quality Assurance Health Equity Accreditation
UnitedHealthcare of California’s commercial HMO plan has been awarded Health Equity Accreditation by the National Committee for Quality Assurance (NCQA), a private, nonprofit organization dedicated to improving health care quality.
UnitedHealthcare Launches Program to Address Type 2 Diabetes in Owensboro Community
UnitedHealthcare Catalyst, a community-based program that uses data to tackle the highest-priority health challenges in local communities, has just launched in Owensboro, Kentucky, with a focus on type 2 diabetes.
UnitedHealth Group Reports Fourth Quarter and Full Year 2023 Financial Results
UnitedHealth Group (NYSE: UNH) reported full year and fourth quarter 2023 results reflecting broad-based growth at Optum and UnitedHealthcare.
UNITEDHEALTH GROUP ANNOUNCES EARNINGS RELEASE DATE
UnitedHealth Group (NYSE: UNH) will release its fourth quarter and full year 2023 financial results on Friday, January 12, 2024, before the market opens, and will host a teleconference at 8:45 a.m. ET to discuss the results with analysts and investors.
Optum Rx Offers New Weight Management Program
Optum Rx, a pharmacy care services company, has launched Optum Rx Weight Engage, a comprehensive weight management and wellness support program. Optum Rx Weight Engage will be available to consumers of plan sponsors, including employers, beginning Jan. 1, 2024.
UnitedHealth Group Named to the Dow Jones Sustainability North America and World Indices for 25th Consecutive Year
UnitedHealth Group has been named to the Dow Jones Sustainability North America Index and the Dow Jones Sustainability World Index for 2023 in the Health Care Providers & Services Industry
UnitedHealthcare Community Plan of Arizona Selected To Continue Serving Arizona Long Term Care System (ALTCS) Elderly/Physical Disability (EPD) Members
Arizona Health Care Cost Containment System (AHCCCS), the state’s Medicaid agency, has announced its intention to award UnitedHealthcare Community Plan of Arizona as one of two organizations to administer its Arizona Long Term Care System (ALTCS) EPD program for individuals who are elderly and/or have a physical disability.
UnitedHealth Group Updates Business Outlook Ahead of Investor Conference
UnitedHealth Group (NYSE: UNH) issued financial guidance ahead of its annual Investor Conference which takes place on November 29, beginning at 8:00 a.m. ET.
UnitedHealth Group to Host 2023 Investor Conference
UnitedHealth Group will host its annual Investor Conference with analysts and institutional investors in New York City on Wednesday, November 29, 2023, beginning at 8:00 a.m. ET.
UnitedHealthcare Community Plan of Rhode Island Awarded NCQA Health Equity Accreditation
UnitedHealthcare Community Plan of Rhode Island has been awarded Health Equity Accreditation by the National Committee for Quality Assurance (NCQA), a private, nonprofit organization dedicated to improving health care quality.
UnitedHealthcare Provides $200,000 to Six Organizations Supporting Youth in North Carolina
UnitedHealthcare Community Plan of North Carolina has announced $200,000 in grant funding to six local organizations supporting children in foster care and transition age youth across the state.
Optum Rx Takes Additional Steps to Lower the Cost of Insulin
Optum Rx, a pharmacy services company, today announced additional actions to make insulin more affordable, moving several rapid-, short- and long-acting insulins to tier one, which offers the lowest cash price consumers pay.
UnitedHealth Group Board Authorizes Payment of Quarterly Dividend
The UnitedHealth Group board of directors has authorized payment of a cash dividend of $1.88 per share, to be paid on December 12, 2023, to all shareholders of record of UNH common stock as of the close of business December 4, 2023.
Charlie Baker Joins UnitedHealth Group’s Board of Directors
UnitedHealth Group announced Charlie Baker, the former governor of Massachusetts and a prominent former health care executive, has been appointed to its Board of Directors, effective immediately.
United Health Foundation Awards $2.3 Million Grant to Mary Bird Perkins Cancer Center to Increase Cancer Services in Underserved Communities
The United Health Foundation today announced a three-year, $2.3 million grant partnership with Mary Bird Perkins Cancer Center to help increase access to prostate and colorectal cancer education, screening and support for historically underserved individuals across Louisiana
UnitedHealthcare to Offer Individual and Family Plans on the Health Insurance Marketplace in 26 States for 2024
UnitedHealthcare announced its 2024 Individual and Family ACA Marketplace Plans, which feature affordable coverage, convenient access to care and a wide range of benefits in 26 states.
Optum Rx Opens New Integrated Pharmacy in Arizona
Optum Rx opened a state-of-the-art home delivery pharmacy today in Mesa, Arizona.
UnitedHealthcare Community Plan of Kentucky Awarded NCQA Health Equity Accreditation
UnitedHealthcare Community Plan of Kentucky has earned Health Equity Accreditation status by the National Committee for Quality Assurance (NCQA).
UnitedHealth Group Reports Third Quarter Results
UnitedHealth Group (NYSE: UNH) reported third quarter 2023 performance led by broad-based growth at Optum and UnitedHealthcare.
UnitedHealthcare’s Surest Leads to More Preventive Care, Improves Member Satisfaction and Lowers Costs, Data Shows
ProHealth Care and Optum Launch Strategic Relationship to Enhance the Health Care Experience for ProHealth Patients
ProHealth Care and Optum have entered into a strategic relationship to enhance patient care, deliver innovative technology solutions and help ProHealth Care maintain its focus on serving patients and the community.
UnitedHealthcare’s 2024 Medicare Advantage Plans Offer Enhancements to Benefits that Matter Most to Members
UnitedHealthcare® today introduced its 2024 Medicare Advantage plans, delivering a simpler member experience with enhanced benefits, broad network access and cost-savings through valuable specialty and prescription drug coverage.
UNITEDHEALTH GROUP ANNOUNCES EARNINGS RELEASE DATE
UnitedHealth Group will release its third quarter 2023 financial results on Friday, October 13, 2023, before the market opens, and will host a teleconference at 8:45 a.m. ET to discuss the results with analysts and investors.
UnitedHealthcare Selected by Texas Health and Human Services Commission To Serve STAR+PLUS Beneficiaries
The Texas Health and Human Services Commission has selected UnitedHealthcare Community Plan of Texas as one of the seven managed care organizations to administer the Medicaid managed care program STAR+PLUS.
UnitedHealthcare Awards $500,000 to Five Federally Qualified Health Centers To Increase Access To Behavioral Health Services
UnitedHealthcare Community Plan of Michigan awarded five federally qualified health centers (FQHCs) $100,000 grants to expand access to behavioral health services across the state.
UnitedHealth Group Board Authorizes Payment of Quarterly Dividend
The UnitedHealth Group (NYSE: UNH) board of directors has authorized payment of a cash dividend of $1.88 per share, to be paid on September 19, 2023, to all shareholders of record of UNH common stock as of the close of business September 11, 2023.
UnitedHealthcare Selected by New Mexico Human Services Department To Serve Medicaid Members via Turquoise Care
The New Mexico Human Services Department has announced its intention to award UnitedHealthcare as one of four organizations to administer Turquoise Care, the state’s Medicaid program, statewide.
UnitedHealthcare Donates $2.85 Million To Help Health Service Workers Better Care For Indiana’s Seniors
UnitedHealthcare Community Plan of Indiana has provided $2.85 million to four organizations working to advance the direct service health workforce in the state.
Optum and Capella University Announce New Nurse Practitioner Program To Address the Growing National Need for Skilled Clinicians
Optum, a diversified health services company, and Capella University, an accredited online university, announced a new educational program designed to address the growing need for skilled, advanced practice nurses.
UnitedHealthcare Community Plan of Ohio Awarded NCQA Health Equity Accreditation
UnitedHealthcare Community Plan of Ohio announced it was awarded Health Equity Accreditation by the National Committee for Quality Assurance, a private, nonprofit organization dedicated to improving health care quality.
UnitedHealthcare Donates $11 Million to Community Organizations Through Its Empowering Health Program
UnitedHealthcare is donating $11 million in grants through its Empowering Health program to community-based organizations across 12 states.
UnitedHealth Group Reports Second Quarter Results
Strong and well-balanced growth continued across UnitedHealth Group (NYSE: UNH) in the second quarter of 2023.
Optum Rx Expands Choice, Improves Affordability for Patients With Two Additional HUMIRA Biosimilars
Starting July 1, clients of Optum Rx will have access to three biosimilar alternatives for HUMIRA, a highly utilized biologic medication used in the treatment of autoimmune diseases.
UnitedHealthcare Community Plan of Arizona Awarded NCQA’s Health Plan Accreditation and Long-Term Services & Supports Distinction
UnitedHealthcare Community Plan of Arizona has been awarded the industry-recognized Health Plan Accreditation and Long-Term Services and Supports Distinction by the National Committee for Quality Assurance.
UnitedHealthcare Catalyst Aims To Improve Health Outcomes for Individuals With Diabetes in Southwest Georgia
UnitedHealthcare Catalyst, a community-based program that leverages data to drive better health, will launch in Southwest Georgia.
UnitedHealthcare Community Plan of Mississippi Recognized With NCQA Health Equity Accreditation
UnitedHealthcare Community Plan of Mississippi has been awarded Health Equity Accreditation status by the National Committee for Quality Assurance.
UnitedHealth Group’s 2022 Sustainability Report Highlights Efforts To Diversify the Health Workforce, Minimize Its Environmental Footprint
UnitedHealth Group published its 2022 Sustainability Report, which details progress toward long-term commitments along with efforts to help meet the needs of those it serves, including customers, employees, shareholders and society broadly.
UnitedHealth Group Increases Dividend; Announces Annual Shareholder Meeting Results
UnitedHealth Group announced an increase to its dividend and provided an update on its 2023 annual shareholder meeting.
Optum Offers To Combine With Amedisys, Advancing Value-Based Care for Patients
Optum, a diversified health services company, has submitted an all-cash proposal to the Board of Directors of Amedisys, a leading provider of home health, hospice and high-acuity care, to combine with Amedisys.
UnitedHealthcare Provides $275,000 to Three North Carolina Nonprofits To Improve Health Outcomes for Children
UnitedHealthcare Community Plan of North Carolina has announced $275,000 in grant funding to three local organizations supporting children in kinship and foster care across the state.
UnitedHealth Group Reports First Quarter 2023 Results
UnitedHealth Group (NYSE: UNH) reported first quarter 2023 results reflecting consistent broad-based growth at Optum and UnitedHealthcare.
United Health Foundation Awards $2 Million Grant to Rainbow Health To Increase Access to Mental Health Care for LGBTQ+ and BIPOC Youth
The United Health Foundation, the philanthropic foundation of UnitedHealth Group (NYSE: UNH), today announced a three-year, $2 million grant partnership to address disparities related to suicide, depression and anxiety among LGBTQ+ and BIPOC youth and young adults ages 14-25 in Minnesota.
UnitedHealth Group Announces Earnings Release Date
UnitedHealth Group (NYSE: UNH) will release its first quarter 2023 financial results on Friday, April 14, 2023, before the market opens, and will host a teleconference at 8:45 a.m. ET to discuss the results with analysts and investors.
New Data: College Students More Likely to Self-Report High-Risk Mental and Behavioral Health Concerns Than Parents Perceive
UnitedHealthcare announced new survey findings revealing college students are more likely to report they or a roommate or friend have encountered mental or behavioral health concerns over the past year.
UnitedHealthcare Recommended by the State of Indiana To Serve Its Managed Long-Term Services and Supports Medicaid Beneficiaries
UnitedHealthcare Community Plan of Indiana has been recommended by the state of Indiana, Family and Social Services Administration, as one of four managed care organizations to administer its Pathways for Aging (Pathways) program.
UnitedHealthcare Awards $95,000 Workforce Development Grant to Step Up Savannah To Increase Access to Employment Resources
UnitedHealthcare Community Plan of Georgia has awarded a $95,000 grant to Step Up Savannah. The grant will support the Chatham Apprentice Program (CAP), a workforce development and resource program working to address multi-generational poverty in Chatham and surrounding counties.
UnitedHealthcare Community Plan of Wisconsin Awarded NCQA Health Equity Accreditation
UnitedHealthcare Community Plan of Wisconsin was awarded Health Equity Accreditation by the National Committee for Quality Assurance (NCQA).
UnitedHealth Group Board Authorizes Payment of Quarterly Dividend
The UnitedHealth Group (NYSE: UNH) board of directors has authorized payment of a cash dividend of $1.65 per share, to be paid March 21, 2023, to common stock shareholders of record as of the close of business March 13, 2023.
United Health Foundation Awards $3.2 Million Grant to East Carolina University To Improve Youth Mental Health
The United Health Foundation, the philanthropic foundation of UnitedHealth Group (NYSE: UNH), today announced a three-year, $3.2 million grant partnership with East Carolina University (ECU).
UnitedHealthcare Introduces New Rewards Program With a Modern Approach to Well-Being
UnitedHealthcare has introduced UnitedHealthcare Rewards, a new rewards program in which eligible members, including spouses, can use wearable devices to earn up to $1,000 each per year by completing various daily health goals and one-time activities.
UnitedHealthcare Provides $750,000 Grant to Community Health Care Association of New York State To Create Program That Aims To Improve Health Equity
UnitedHealthcare Community Plan of New York has announced a $750,000 investment to support a grant program in collaboration with the Community Health Care Association of New York State (CHCANYS).
United Health Foundation Awards $3 Million Grant to Children’s Minnesota To Address Health Disparities
The United Health Foundation, the philanthropic foundation of UnitedHealth Group (NYSE: UNH), and Children’s Minnesota today announced a three-year, $3 million grant partnership to address pediatric disparities related to asthma, vaccinations and mental health for underserved children and families in the Twin Cities.
UnitedHealth Group Invests $10 Million in New Fund, Invest Appalachia, to Address Social Needs and Advance Economic Equity
UnitedHealth Group has committed $10 million as a lead investor in the first round of the Invest Appalachia (IA) Fund, a regional initiative launched to accelerate funding in community development across Appalachian counties in Kentucky, North Carolina, Ohio, Tennessee, Virginia and West Virginia.
Optum Rx Launches Price Edge to Automatically Provide Members the Best Available Prescription Drug Price
Optum Rx has launched Price Edge, a tool that seamlessly compares available direct-to-consumer pricing for traditional generic drugs with insurance pricing to ensure members always get the lowest prescription drug price.
UnitedHealthcare Expands Suite of Behavioral Health Offerings With Virtual Behavioral Coaching
More than 5 million UnitedHealthcare® commercial members now have access to virtual behavioral coaching at no added cost.
UnitedHealth Group Reports Fourth Quarter and Full Year 2022 Financial Results
UnitedHealth Group (NYSE: UNH) reported full year and fourth quarter 2022 results reflecting broad-based growth at Optum and UnitedHealthcare.
Owensboro Health and Optum Launch Comprehensive Partnership to Enhance Patient Care and Experience in Western Kentucky and Southern Indiana
Owensboro Health and Optum today announced a partnership to enhance patient care and experience while meeting the community’s evolving health care needs.
Northern Light Health and Optum Launch Strategic Relationship to Enhance the Health Care Experience
Northern Light Health and Optum today announced a strategic relationship to enhance the health care experience for patients and providers throughout Maine.
New Mexico Organizations Improving Community Health Receive Over $1.1 Million From UnitedHealthcare To Expand Programs
UnitedHealth Group Announces Earnings Release Date
UnitedHealth Group (NYSE: UNH) will release its fourth quarter and full year 2022 financial results on Friday, January 13, 2023, before the market opens, and will host a teleconference at 8:45 a.m. ET to discuss the results with analysts and investors.
Kristen Gil Joins UnitedHealth Group Board of Directors
UnitedHealth Group (NYSE: UNH) announced Kristen Gil of Alphabet Inc. (NASDAQ: GOOG) has been appointed to its Board of Directors, effective immediately.
UnitedHealth Group Named to the Dow Jones Sustainability North America and World Indices for 24th Consecutive Year
UnitedHealth Group (NYSE: UNH) has been named to the Dow Jones Sustainability North America Index and the Dow Jones Sustainability World Index for 2022 in the Health Care Providers & Services Industry Group. It is the 24th consecutive year that UnitedHealth Group has been named to the indices, beginning in 1999 when the rankings were established.
United Health Foundation Launches $3.1 Million Partnership with American Nurses Foundation to Fight Nurse Burnout and Attrition
The United Health Foundation, the philanthropic foundation of UnitedHealth Group (NYSE: UNH), today announced a three-year, $3.1 million grant partnership with the American Nurses Foundation to fight nurse burnout through implementation of the Building Blocks for Beating Burnout (B4) program.
UnitedHealth Group Updates Business Outlook Ahead of Investor Conference
UnitedHealth Group (NYSE: UNH) issued financial guidance ahead of its annual Investor Conference which takes place on November 29, beginning at 8:00 a.m. ET.
UnitedHealth Group to Host 2022 Investor Conference
UnitedHealth Group will host its annual Investor Conference with analysts and institutional investors in New York City on Tuesday, November 29, 2022, beginning at 8:00 a.m. ET.
UnitedHealthcare to Provide Millions of Eligible Medicare Members Access to All Life Time Clubs Nationwide
UnitedHealthcare, part of UnitedHealth Group (NYSE: UNH) and Life Time (NYSE: LTH), the nation's premier healthy lifestyle brand, have expanded their relationship to include access to all Life Time locations, helping even more people stay active and improve physical and mental well-being.

UnitedHealthcare to Help Millions of AARP Members Save on Hearing Aids
UnitedHealthcare is now administering AARP Hearing Solutions, helping make it easier and more affordable for millions of Americans to purchase prescription and over-the-counter (OTC) hearing aids.
UnitedHealth Group Board Authorizes Payment of Quarterly Dividend
The UnitedHealth Group (NYSE: UNH) board of directors has authorized payment of a cash dividend of $1.65 per share, to be paid December 13, 2022, to common stock shareholders of record as of the close of business December 5, 2022.
UnitedHealthcare Expands Its Individual and Family Plan Footprint
UnitedHealthcare today announced its 2023 Individual and Family Plans in the Health Insurance Marketplace, which will feature affordable coverage, a wide range of benefits, and a simple service experience in 22 states.
UnitedHealthcare Community Plan of Florida Awarded NCQA Health Equity Accreditation
The National Committee for Quality Assurance (NCQA) awarded UnitedHealthcare Community Plan of Florida with its Health Equity Accreditation.
UnitedHealthcare Awards More Than $180,000 in Community Grants to Support Behavioral and Maternal Health in New Mexico
As part of an ongoing effort to address vital social determinants of health across New Mexico, UnitedHealthcare has awarded three New Mexico-based organizations $188,000 in community grants to address behavioral and maternal health in local communities.
UnitedHealthcare Invests $5 Million in Morgan’s Wonderland to Promote Health and Employment Equity for Individuals With Disabilities
This funding will enable the new Multi-Assistance Center at Morgan's Wonderland to implement a Practice Without Pressure program and an Employment Support Center for individuals with disabilities
UnitedHealth Group Reports Third Quarter 2022 Results
Strong and well-balanced performance continued across UnitedHealth Group (NYSE: UNH) in the third quarter of 2022.
United Health Foundation Launches $3 Million Partnership with Active Minds to Help Address The Youth Mental Health Crisis
Three-year commitment will address increases in youth mental health challenges revealed by the 2022 America’s Health Rankings® Health of Women and Children Report.
United Health Foundation Donates $1 Million to Support Residents of Florida Affected by Hurricane Ian
The United Health Foundation, the philanthropic foundation of UnitedHealth Group (NYSE:UNH) – the parent company of UnitedHealthcare and Optum – is donating $1 million to help residents of Florida address urgent response needs following Hurricane Ian.
Optum and Change Healthcare Complete Combination
The combined businesses share a vision for achieving a simpler, more intelligent and adaptive health system for patients, payers and care providers.
United Health Foundation Donates $200,000 to Support Residents of Puerto Rico Affected by Hurricane Fiona
The United Health Foundation, the philanthropic foundation of UnitedHealth Group (NYSE:UNH) – the parent company of UnitedHealthcare and Optum – is donating $200,000 to help residents of Puerto Rico in their ongoing recovery and rebuild following Hurricane Fiona.
UnitedHealthcare Awards Community Grants in New Mexico to Address Social Determinants of Health
UnitedHealthcare Selected by Nebraska Department of Health and Human Services to Serve Medicaid Beneficiaries
Nebraska residents who qualify for Medicaid coverage will continue to have access to UnitedHealthcare’s comprehensive care and preventive health and wellness programs
UnitedHealthcare and Peloton to Provide Millions of More People With Access to a Leading Interactive Fitness Platform
UnitedHealthcare, part of UnitedHealth Group (NYSE: UNH), and Peloton Interactive, Inc. (Nasdaq: PTON) have renewed and expanded their relationship to help more people get or stay active and improve their overall well-being.
UnitedHealth Group Announces Earnings Release Date
UnitedHealth Group (NYSE: UNH) will release its third quarter 2022 financial results on Friday, October 14, 2022, before the market opens, and will host a teleconference at 8:45 a.m. ET to discuss the results with analysts and investors.
Walmart and UnitedHealth Group Collaborate to Deliver Access to High-Quality, Affordable Health Care
Today, Walmart Inc. (NYSE: WMT) and UnitedHealth Group (NYSE: UNH) announced the beginning of an initial 10-year, wide-ranging collaboration, bringing together the collective expertise of both companies in serving millions of people with high-quality, affordable health services that improve health outcomes and improve the patient experience.
UnitedHealthcare and Sesame Workshop Celebrate Grandparents Day With New Resources to Help Families Grow in Healthy Ways
UnitedHealthcare and Sesame Workshop, the nonprofit educational organization behind Sesame Street, are celebrating National Grandparents Day on Sept. 11 with a new resource, Happy, Healthy, Hopeful: Stretching Our Food Dollars.
UnitedHealth Group Board Authorizes Payment of Quarterly Dividend
The UnitedHealth Group board of directors has authorized payment of a cash dividend of $1.65 per share.

UnitedHealthcare’s Surest Offers a New Approach to Health Insurance
Surest™, formerly Bind, offers a new approach to health benefits that eliminates deductibles and offers access to clear, upfront pricing information before people access care
UnitedHealthcare and Optum Donate $205,000 to Support Eastern Kentucky Communities Devastated by Recent Flooding
UnitedHealthcare and Optum announced today a $205,000 donation to help eastern Kentucky residents following the devastating flooding that impacted local communities.
Optum to Offer Lower-Cost Insulin for Uninsured People Living With Diabetes on Optum Store
Optum is working with Sanofi to offer a 30-day supply of commonly used Sanofi insulins for $35 to people with diabetes who do not have insurance through its online health services and products retailer Optum Store.
Consumers Want Better Digital Tools for Finding Health Care: Survey
A growing number of health care consumers prefer more seamless digital experiences in scheduling and interacting with their health care provider and health plan.
UnitedHealth Group Reports Second Quarter Results
UnitedHealth Group (NYSE: UNH) reported second quarter 2022 performance led by broad-based growth at Optum and UnitedHealthcare.
UnitedHealthcare To Eliminate Out-of-Pocket Costs on Several Prescription Drugs, Including Insulin, for Eligible Members
UnitedHealthcare will eliminate out-of-pocket costs in standard fully insured group plans for certain preferred prescription drugs, including insulin and several drugs used to treat emergencies such as severe allergic reactions, hypoglycemia, opioid overdoses, and acute asthma attacks.
UnitedHealth Group Commits $25 Million to New England Healthy Neighborhoods Fund
UnitedHealth Group (NYSE: UNH) today announced a $25 million commitment to the Healthy Neighborhoods Equity Fund II (HNEF II).
UnitedHealthcare Supports African American Babies Coalition Addressing Racial Health Disparities in Minneapolis-St. Paul With $150,000 Grant
UnitedHealthcare, a UnitedHealth Group company, awarded a $150,000 grant to the African American Babies Coalition and Projects (Wilder AABC) in support of its initiatives to educate the community, recruit child care professionals and develop programs for African American families in the Twin Cities.
Optum Launches Laboratory Benefit Management Solution to Reduce Unnecessary Testing and Improve Quality of Care
Optum today announced the launch of a comprehensive laboratory benefit management solution designed to help health plans reduce unnecessary lab testing and ensure their members receive appropriate, high-quality tests.
UnitedHealth Group 2021 Sustainability Report Includes New Health Equity and Environmental Health Commitments
UnitedHealth Group today released its 2021 Sustainability Report detailing the company’s ongoing commitment to helping meet the needs of those it serves, including customers, employees, shareholders and society broadly.
The United Health Foundation Commits $100 Million to Further Advance a Diverse Health Workforce
The United Health Foundation is making a $100 million commitment over 10 years to advance health equity, furthering its efforts to eliminate health disparities.
UnitedHealth Group Provides Updates on Annual Shareholder Meeting, Board Actions
UnitedHealth Group provided updates on its 2022 annual shareholder meeting and actions by its Board of Directors.
UnitedHealth Group Announces Earnings Release Date
UnitedHealth Group will release its second quarter 2022 financial results on Friday, July 15, 2022, before the market opens.
UnitedHealthcare Selected by State of Missouri to Serve Medicaid Beneficiaries
The state of Missouri has selected UnitedHealthcare Community Plan of Missouri as one of three managed care organizations to administer its MO HealthNet Managed Care Program for Medicaid members in Temporary Assistance for Needy Families (TANF) and the Children’s Health Insurance Program (CHIP).
Optum Rx Donates COVID-19 Test Kits to Increase Access to Free Testing Among Underserved Communities in Chicago
Optum Rx, the pharmacy care services business of UnitedHealth Group, is donating 5,000 at-home COVID-19 rapid antigen self-tests to increase access to COVID-19 testing and support for underserved communities across Chicago.
UnitedHealth Group Reports First Quarter 2022 Results
Strong and well-balanced growth continued across UnitedHealth Group (NYSE: UNH) in the first quarter of 2022.
UnitedHealthcare to Address Maternal Health Outcomes, Access to Care and Health Equity With Doula Program Expansion Into Western North Carolina
UnitedHealthcare, Mountain Area Health Education Center (MAHEC) and SistasCaring4Sistas (SC4S) announced the expansion of a community-based doula program into western North Carolina.
Additional $100 Million Investment in Housing Bolsters UnitedHealth Group’s Efforts to Address Social Determinants and Achieve Better Health Outcomes
UnitedHealth Group announced an additional $100 million investment in the Health & Housing Fund — a partnership with Stewards of Affordable Housing for the Future (SAHF) and National Affordable Housing Trust (NAHT).
Change Healthcare and Optum Extend Merger Agreement
Optum, a diversified health services company, and Change Healthcare (NASDAQ: CHNG), a health care technology leader, have agreed to extend their merger agreement to December 31, 2022.
Optum and LHC Group to Combine, Advancing Abilities to Extend Value-Based Care into Patients’ Homes
Optum, a diversified health services company, and LHC Group (NASDAQ: LHCG), a national patient-focused provider of high-quality in-home health care services, have agreed to combine to further strengthen their shared ability to advance value-based care.
UnitedHealth Group Announces Earnings Release Date
UnitedHealth Group will release its first quarter 2022 financial results on Thursday, April 14, 2022.
UnitedHealthcare Provides Nearly $170K to the University of Mississippi Medical Center to Support Children’s Health
UnitedHealthcare Community Plan of Mississippi has provided $169,500 in funding to the University of Mississippi Medical Center to support children, their families, and the provider community with local professional sickle cell disease expertise and behavioral health support and services.
Telehealth Use Will Outlive the Pandemic for Health Care Providers, Survey Shows
Health care providers are planning for patient access to virtual care that outlasts the pandemic, according to a survey Optum released.
United Health Foundation Invests in Indiana Nonprofit to Expand Access to Comprehensive Health Care for Rural and Low-Income Communities
The United Health Foundatio has awarded a $2 million, three-year grant to HealthNet Inc., a nonprofit health care provider serving Indiana, to expand access to primary and behavioral health care in Morgan and Monroe counties in Indiana, as well as high-poverty areas in Indianapolis.
United Health Foundation to Provide $1M to Support Relief Efforts in Ukraine
The United Health Foundation, the philanthropic foundation of UnitedHealth Group (NYSE: UNH), today announced a $1 million donation to support relief efforts in Ukraine.
Optum Launches Specialty Fusion to Simplify Specialty Care and Lower Costs
Optum today announced the launch of Optum® Specialty Fusion™, a first-of-its-kind specialty medication management solution, to simplify care for patients with complex conditions and lower the cost of expensive specialty drugs.
UnitedHealth Group Board Authorizes Payment of Quarterly Dividend
The UnitedHealth Group (NYSE: UNH) board of directors has authorized payment of a cash dividend of $1.45 per share, to be paid on March 22, 2022, to all shareholders of record of UnitedHealth Group common stock as of the close of business on March 14, 2022.
District of Columbia Selects UnitedHealthcare to Administer District Dual Choice Program
The District of Columbia (the district) has selected UnitedHealthcare to administer its District Dual Choice program.
UnitedHealthcare Dental Launches Digital Resources, Collaboration with quip, to Help Improve Dental Care
UnitedHealthcare Dental has introduced several enhancements designed to help people improve their oral health and access dental care in a more convenient and informed way.
UnitedHealthcare Invests $550,000 in the Mississippi Public Health Institute to Improve Maternal Health Equity and Outcomes
UnitedHealthcare Community Plan of Mississippi today announced a $550,000 investment in the Mississippi Public Health Institute (MSPHI), a nonprofit entity established to protect and improve the health and well-being of Mississippians.
Optum Idaho Donates $200,000 To Increase Mental Health Care Access Statewide
Optum Idaho, the managed care organization for the state of Idaho’s Medicaid behavioral health plan and part of UnitedHealth Group (NYSE: UNH), has awarded $200,000 to the University of Idaho’s Project ECHO (Extension for Community Healthcare Outcomes) aimed at increasing mental health care access statewide for adults, children and families.
MarinHealth and Optum Launch New Strategic Relationship to Streamline Administrative Functions and Improve the Patient Experience in Marin County, California
MarinHealth Medical Center and Optum today announced a strategic relationship to advance MarinHealth’s operational objectives and support MarinHealth’s continued commitment to providing high-quality, affordable, convenient and accessible care for North Bay residents.
Sesame Workshop Launches New Resources to Help Children and Families Build a Lifelong Foundation of Resilience
With support from UnitedHealthcare, free online courses for providers and digital storybooks for children build upon Sesame Workshop’s ongoing commitment to building happy and healthy communities
UnitedHealth Group Reports Fourth Quarter and Full Year 2021 Financial Results
UnitedHealth Group (NYSE: UNH) reported full year and fourth quarter 2021 results led by continued broad-based growth across the enterprise.
UnitedHealthcare Awards Community Grants to Three Organizations Focused on Improving Health Equity and Addressing Social Determinants in Michigan
UnitedHealthcare Community Plan of Michigan has awarded $75,000 in community grants to three organizations focused on improving maternal and infant health outcomes and combating addiction in Michigan.
UnitedHealthcare Enhances Eye Care Program by Helping Reduce People’s Exposure to Blue Light
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, is investing in new ways to help children and adults across the country reduce their exposure to blue light and support their overall eye health, amid ongoing use of screens during COVID-19 and the greater reliance on remote school and work.
AI Survey: Health Care Organizations Continue to Adopt Artificial Intelligence to Help Achieve Better, More Equitable and Affordable Patient Outcomes
Survey respondents overwhelmingly agree health care organizations have a higher duty than organizations in other industries to ensure responsible use of AI.
United Health Foundation Donates $500,000 to Support Kentucky Communities Devastated by Recent Tornadoes
The United Health Foundation announced today a $500,000 donation to help Kentucky residents recover and rebuild following the devastating tornadoes that struck local communities this past weekend.
UnitedHealth Group Donates $300,000 to YouthZone to Support Teen Mental Health Across Colorado’s Western Slope in Collaboration With the Colorado Attorney General’s Office
Rocky Mountain Health Plans, a UnitedHealth Group company, is donating $300,000 to YouthZone to foster positive youth development for teens across Colorado’s Western Slope.
UnitedHealthcare Community Plan of California to Address Health Equity and Expand Access to Health Care With Investments in 17 San Diego-Based Organizations
UnitedHealthcare Community Plan of California today announced a $1.5 million investment in community-based programs aimed to reduce health disparities and improve health equity in San Diego.
America’s Health Rankings 2021 Annual Report Illustrates Complex Picture of America’s Health
The United Health Foundation, the philanthropic foundation of UnitedHealth Group (NYSE: UNH), today released its “America’s Health Rankings® 2021 Annual Report,” which provides insights into the early effects of COVID-19 on Americans’ health and well-being.
UnitedHealthcare Introduces Health Plan Delivering Lower Costs and a Patient-Focused Health Care Experience
UnitedHealthcare has introduced a new health plan that offers consumers in Southwest Arizona personalized and seamless customer support as well as the opportunity to save up to 15% on premiums.
UnitedHealth Group Updates Business Outlook Ahead of Investor Conference
UnitedHealth Group issued financial guidance ahead of its annual Investor Conference which takes place on November 30, beginning at 8 a.m. ET.
UnitedHealthcare to Offer Comprehensive Massachusetts One Care Benefit Plan
UnitedHealthcare Community Plan of Massachusetts is now offering One Care for people eligible for both Medicare and MassHealth living in Bristol, Hampden, Plymouth, Suffolk, Worcester, Hampshire, Franklin, and Middlesex counties and parts of Essex County.
UnitedHealthcare Community Plan of Rhode Island Provided $110,000 to Support Children’s Health
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, has provided $110,000 in investments in the past several months to community-based organizations in Rhode Island to support children and their families with health education, advocacy and healthy meals.
UnitedHealth Group to Host 2021 Investor Conference
UnitedHealth Group will host its annual Investor Conference with analysts and institutional investors in New York City on Tuesday, November 30, 2021, beginning at 8:00 a.m. ET.
United Health Foundation Partners With Harris-Stowe State University to Create New Bioinformatics Program
The United Health Foundation, the philanthropic foundation of UnitedHealth Group (NYSE: UNH), has awarded a $2 million, three-year grant to Harris-Stowe State University to create a bioinformatics program for undergraduate students at the historically Black university located in St. Louis.
UnitedHealth Group Included in the Dow Jones Sustainability North America and World Indices for 23rd Consecutive Year
UnitedHealth Group (NYSE: UNH) has been named to the Dow Jones Sustainability North America Index and the Dow Jones Sustainability World Index for 2021 in the Health Care Equipment and Services Industry Group.

A Record Number of Americans Surveyed Say They Are Prepared to Select a Health Plan During Open Enrollment
Most Americans said they are prepared to select a health plan during this year’s open enrollment season, while the COVID-19 pandemic continues to spur interest in virtual care for medical services and digital fitness apps to help people pursue at-home fitness routines.
United Health Foundation Grant to Children’s National Hospital to Address Health Needs of Youth in Communities With Fewer Resources
The United Health Foundation, the philanthropic foundation of UnitedHealth Group (NYSE: UNH), has awarded a three-year, $3.4 million grant to Children’s National Hospital to improve access to health care for school-aged children in Washington, D.C.’s most under-resourced communities.
UnitedHealth Group Board Authorizes Payment of Quarterly Dividend
The UnitedHealth Group (NYSE: UNH) board of directors has authorized payment of a cash dividend of $1.45 per share, to be paid on December 14, 2021, to all shareholders of record of UnitedHealth Group common stock as of the close of business on December 6, 2021.
Minnesota Department of Human Services Chooses UnitedHealthcare to Serve Individuals Covered by Medicaid
The Minnesota Department of Human Services, which is partnering with managed care health plans to improve the health and wellness of individuals, selected UnitedHealthcare Community Plan of Minnesota to administer its Medicaid program, effective January 1, 2022.
2022 Individual and Family Plans From UnitedHealthcare Are Available on the Health Insurance Marketplaces in 18 States Offering New, Affordable Benefits
UnitedHealthcare® today announced its 2022 Individual and Family plans, which feature affordable coverage, new benefits, and a simplified enrollment and member service experience.
UnitedHealthcare and UWH of North Carolina to Address Maternal Health Needs With Group Prenatal Care Initiative
UnitedHealthcare and UWH of North Carolina, an affiliated medical practice of Unified Women’s Healthcare, today announced an initiative using the group prenatal care model, CenteringPregnancy, to improve outcomes and reduce racial and social disparities among mothers in North Carolina by providing access to quality maternal care.
UnitedHealthcare Community Plan of Missouri Awards $500,000 to Address Health Equity
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, has awarded $500,000 in grants to community-based organizations in Missouri to expand access to care, support maternal and child health and address the social determinants of health for individuals and underserved communities.
UnitedHealthcare to Launch New Virtual-First Health Plan to Help People Access a Dedicated Care Team 24/7 and Obtain Quality Care at a Lower Cost
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, announced the launch of NavigateNOW, a virtual-first health plan that offers an integrated approach to provide care both virtually and in-person.
UnitedHealth Group Reports Third Quarter 2021 Performance
Consistent, well-balanced growth continued across UnitedHealth Group (NYSE: UNH) in the third quarter 2021.
SSM Health and Optum Launch Innovative Collaboration to Make Quality Care More Accessible and Affordable
SSM Health and Optum, a subsidiary of UnitedHealth Group (NYSE: UNH), announced an innovative collaboration focused on making quality care more accessible and affordable for people across the Midwest.
UnitedHealthcare’s 2022 Medicare Plans Shaped by Consumer Expectations for Value, Choice and Experience
UnitedHealthcare® today introduced its 2022 Medicare Advantage and prescription drug plans, offering expanded access to plans with differentiated value, simple and affordable benefit design and an unparalleled member experience – all defined by what consumers say matters to them most.
Genoa Healthcare Opens 600th Pharmacy Serving Community Mental Health Needs
Genoa Healthcare, the leading provider of pharmacy services for people with mental illness, substance use disorders, and other complex, chronic conditions, has opened its 600th pharmacy amid a growing need for mental health and addiction services during the COVID-19 pandemic.
UnitedHealthcare to Offer Millions of Members Year-Long Access to Apple Fitness+ at No Additional Cost
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, has expanded its work with Apple to provide millions of members with access — at no additional cost — to Apple Fitness+, the first fitness service built entirely around Apple Watch®.
UnitedHealth Group Announces Earnings Release Date
UnitedHealth Group (NYSE: UNH) will release its third quarter 2021 financial results on Thursday, October 14, 2021, before the market opens, and will host a teleconference at 8:45 a.m. ET to discuss the results with analysts and investors.
UnitedHealth Group Donates $4.5 Million to Advance Health Equity Among Underserved Communities Across Oklahoma
UnitedHealth Group (NYSE: UNH), including the United Health Foundation and UnitedHealthcare, is donating a total of $4.5 million to increase access to health care, improve health outcomes and support communities across Oklahoma.
OptumHealth Education Launches LGBTQ+ Education Program for Providers
OptumHealth Education, in partnership with OutCare Health, has launched an accredited, no-cost, and publicly available education program to teach health care professionals about the unique health care needs and disparities experienced by the LGBTQ+ community.
UnitedHealthcare and Sesame Workshop Celebrate Grandparents Day with New Resources to Help Families Grow in Healthy Ways
UnitedHealthcare and Sesame Workshop, the nonprofit educational organization behind Sesame Street, are celebrating National Grandparents Day on Sept. 12 with a new "Grandparents Are Grand!" guidebook.
United Health Foundation Donates $1 Million to Support Residents of Louisiana Affected by Hurricane Ida
The United Health Foundation, the philanthropic foundation of UnitedHealth Group (NYSE:UNH), along with its UnitedHealthcare and Optum businesses announced today a $1 million donation to help Louisiana residents recover and rebuild following the devastating impact of Hurricane Ida.
State of Nevada Selects UnitedHealthcare to Serve its Medicaid Beneficiaries
The state of Nevada has selected Health Plan of Nevada, a UnitedHealthcare company, as one of four managed care organizations to administer its Medicaid program in the counties of Clark and Washoe, effective Jan. 1, 2022.
UnitedHealth Group Board Authorizes Payment of Quarterly Dividend
The UnitedHealth Group (NYSE: UNH) board of directors has authorized payment of a cash dividend of $1.45 per share, to be paid on September 21, 2021, to all shareholders of record of UnitedHealth Group common stock as of the close of business on September 13, 2021.
UnitedHealthcare and Tennessee Initiative for Perinatal Quality Care Focus on Health Equity in Maternal Health Outcomes
Initiative will address racial disparities by providing maternal hypertension and hemorrhage simulation training in 49 hospitals, and testing remote patient monitoring for expectant mothers through Regional One Health
United Health Foundation Launches $3.3 Million Partnership with North Olympic Healthcare Network to Improve Behavioral Health Care on the Olympic Peninsula
Three-year grant partnership aimed at improving behavioral and primary health care access for students and adults.
Empowering Health Grants Help Expand Access to Care
UnitedHealthcare is awarding $11.4 million in Empowering Health grants across 18 states and the District of Columbia to help address these needs for uninsured individuals and underserved communities.
UnitedHealthcare to Provide Millions of Members with Year-Long Access to the Peloton App
UnitedHealthcare, part of UnitedHealth Group (NYSE:UNH), and Peloton (Nasdaq: PTON) are working together to provide millions of Americans with access — at no additional cost — to classes that can help improve their overall fitness and well-being, the first such relationship between Peloton and a health plan.
UnitedHealth Group Reports Second Quarter Results
Strong and diversified growth continued across UnitedHealth Group (NYSE: UNH) in the second quarter 2021.
UnitedHealthcare Introduces the Use of Predictive Analytics to Expand its Capabilities to Address Social Determinants of Health
UnitedHealthcare has introduced the use of predictive analytics to help improve well-being, lower costs and drive engagement in clinical-intervention programs by addressing social determinants of health for people in some employer-sponsored benefit plans.
Optum Awards $1.4 Million in Maternal Health Grants to Five Community Organizations
Optum has awarded $1.4 million in maternal health grants and will provide pro bono services to five community organizations aimed at improving maternal health outcomes and increasing health care access for underserved populations.
New Health Disparities Report Reveals Urgent Need to Address Maternal Mortality, Mental and Behavioral Health, and Food Insecurity in the U.S.
Widespread health disparities persisted across racial, ethnic, gender, geographic and educational lines before COVID-19 pandemic, according to America’s Health Rankings Health Disparities Report.
UnitedHealth Group Announces Earnings Release Date
UnitedHealth Group (NYSE: UNH) will release its second quarter 2021 financial results on Thursday, July 15, 2021, before the market opens, and will host a teleconference at 8:45 a.m. ET to discuss the results with analysts and investors.
Optum Addresses Clinician Shortage in Hemet and Makes it Easier to Access Health Care Services
New clinic, pharmacy and community center makes it easier for people to get health care services under one roof.
New Optum Mobile Clinic Brings Health Care to Utahns Where They Live and Work
Optum Care Network Utah, a part of information and technology-enabled health services business Optum, is making it easier for patients to receive preventive and wellness care with the launch of its new Optum Mobile Clinic.
Rory McIlroy Helps UnitedHealthcare Launch Effort to Encourage Healthier Habits for Americans and Break a GUINNESS WORLD RECORDS™ Title for the Most Pledges Received for a Health Campaign in One Month
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, is encouraging Americans to make health a priority with the 2021 Step Up for Summer Sweepstakes and World Record Challenge.
UnitedHealth Group Releases 2020 Sustainability Report
UnitedHealth Group (NYSE: UNH) today released its 2020 sustainability report detailing the company’s ongoing commitment to helping ensure it meets the needs of those it serves, including its customers, employees, shareholders and society broadly.
UnitedHealth Group Provides Updates on Annual Shareholder Meeting, Board Actions
UnitedHealth Group (NYSE: UNH) provided updates on its 2021 annual shareholder meeting and actions by its Board of Directors at its regular quarterly meeting.
UnitedHealthcare Awards $275,000 in Maternal Health Grants to Seven Community Organizations in Louisiana
UnitedHealthcare Community Plan of Louisiana has awarded $275,000 in maternal health grants to seven community organizations aimed at improving maternal health outcomes, reducing disparities, and expanding access to care.
United Health Foundation Launches $3 Million Partnership with CAMBA, Inc. to Improve Access to Prenatal Care for Brooklyn’s Most Vulnerable Residents
The United Health Foundation, the philanthropic foundation of UnitedHealth Group (NYSE: UNH), has launched a three-year $3 million partnership with CAMBA, Inc. to help improve access to prenatal care for underserved and homeless women in Brooklyn.
United Health Foundation Partners with Valle del Sol Community Health in Arizona to Improve Children’s Access to Care
The United Health Foundation, the philanthropic foundation of UnitedHealth Group (NYSE: UNH), has committed $3 million to Valle del Sol Community Health to help improve school-age children’s access to integrated health care in underserved communities throughout the greater Phoenix metropolitan area.
Bassett Healthcare Network and Optum Launch Strategic Relationship to Advance Quality Care and Improve Experiences for Patients in Central New York
Bassett Healthcare Network and Optum today announced a strategic collaboration to further enhance Bassett’s clinical and operational performance, and advance delivery of high-quality, convenient and affordable health care for patients across Central New York.
New USMD Cancer Care and Infusion Centers Open to Improve Cancer Care in Dallas-Fort Worth
USMD, a physician-led integrated health care organization that is a part of Optum, a UnitedHealth Group (NYSE: UNH) company, opened three new cancer care and infusion centers to improve cancer care for patients in the Dallas-Fort Worth (DFW) Metroplex.
UnitedHealthcare Introduces First-of-its-Kind Community-Based Collaborative to Improve Health Outcomes and Equity
UnitedHealthcare today announced a community-based initiative, Community Catalyst, that convenes a broad range of community stakeholders to identify and address specific health care needs of members of the community and residents of publicly assisted housing who are often difficult to reach and serve.
UnitedHealthcare To Offer New Post-Discharge Support for Retirees with Employer Group Medicare Advantage Plans
UnitedHealthcare announced it will be launching UnitedHealthcare® Healthy at Home, a new offering designed to help retirees safely transition back home after being discharged from a hospital or skilled nursing facility.
UnitedHealth Group Provides Additional Support to Help Fight COVID-19 in India
UnitedHealth Group (NYSE: UNH), through the United Health Foundation, is donating $1 million (₹7.4 crores) in response to the growing coronavirus crisis in India, which is experiencing an unprecedented public health emergency with record-breaking surges in COVID-19 cases and deaths.
UnitedHealthcare Enhances Integration of Medical and Specialty Benefits, Helping Improve Health Outcomes and Affordability
UnitedHealthcare has introduced various enhancements to its integrated approach to medical and specialty benefits, providing members with a more simplified experience and enabling employers to help improve employee health outcomes, increase productivity and lower costs.
United Health Foundation Launches $2.6 Million Partnership with Touro University Nevada to Improve Maternal Health and Reduce Disparities in Underserved Communities
The United Health Foundation, the philanthropic foundation of UnitedHealth Group (NYSE: UNH), is partnering with Touro University Nevada (Touro) to improve access to high-quality prenatal care for underserved and homeless women in southern Nevada.
UnitedHealth Group Donates $30 Million to Increase Health Care Access for Underserved Communities Across Colorado
Rocky Mountain Health Plans, a UnitedHealth Group company, is donating $30 million to increase access to health care and support communities on the Western Slope and across Colorado.
Ohio Department of Medicaid Chooses UnitedHealthcare to Serve Individuals Covered by Medicaid
The Ohio Department of Medicaid, which is partnering with managed care health plans to improve the health and wellness of individuals, selected UnitedHealthcare Community Plan of Ohio as one of six organizations to administer its reimagined Medicaid program, effective early 2022.
UnitedHealth Group Reports First Quarter Performance
Strong, well-diversified business performance contributed to growth across UnitedHealth Group (NYSE: UNH) in the first quarter 2021, even as the Company continued to support consumers, customers and the broader health system in the pandemic response.
Brian Thompson Named Chief Executive Officer of UnitedHealthcare Unit
Brian Thompson has been named Chief Executive Officer of UnitedHealthcare, the health benefits business of UnitedHealth Group (NYSE: UNH).
State of Hawaii Selects UnitedHealthcare to Serve its Medicaid Beneficiaries
Hawaii Medicaid beneficiaries will continue to have access to UnitedHealthcare’s comprehensive medical, behavioral, prescription drug and related services health plan
UnitedHealthcare Awards $240,000 in Maternal Health Grants to Five Community Organizations in Ohio
UnitedHealthcare Community Plan of Ohio has awarded $240,000 in maternal health grants to five community organizations aimed at improving maternal health outcomes, reducing disparities and expanding access to care.
UnitedHealthcare Awards More Than $276,000 in Maternal Health Grants to Six Community Organizations in Tennessee
UnitedHealthcare Community Plan of Tennessee has awarded more than $276,000 in maternal health grants to six community organizations aimed at improving maternal health outcomes, reducing disparities and expanding access to care.
UnitedHealthcare Awards More than $285,000 in Maternal Health Grants to Eight Community Organizations in Mississippi
UnitedHealthcare Community Plan of Mississippi has awarded more than $285,000 in maternal health grants to eight community organizations aimed at improving maternal health outcomes, reducing disparities and expanding access to care.
Study: Real Appeal Digital Weight Loss Program Demonstrates Significant Medical Cost Savings
A new study from Rally Health, Inc., showed significant medical cost savings associated with its digital therapeutic weight loss program Real Appeal® when compared to a control group of similar individuals.
UnitedHealth Group Announces Earnings Release Date
UnitedHealth Group will release its first quarter 2021 financial results on Thursday, April 15, 2021.
UnitedHealthcare Hearing Launches Virtual Option to Help Plan Participants Remotely Access Hearing Health Care and Treatment
UnitedHealthcare Hearing has introduced a new virtual care option for people across the country and individuals enrolled in eligible UnitedHealthcare employer-sponsored and Medicare Advantage plans, helping expand access to custom-programmed hearing aids and potentially reducing the need for in-person appointments for fittings or adjustments.
UnitedHealth Group Board Authorizes Payment of Quarterly Dividend
The UnitedHealth Group board of directors has authorized payment of a cash dividend of $1.25 per share, to be paid on March 23, 2021.
UnitedHealthcare Children’s Foundation Awards 25,000th Grant
UnitedHealthcare Children’s Foundation (UHCCF) awarded its 25,000th grant, continuing its mission of helping families gain greater access to medical care that improves the quality of life of children across the United States.
UnitedHealth Group Announces Executive Leadership Actions
Sir Andrew Witty has been named chief executive officer succeeding David S. Wichmann, who retires after successfully guiding the company through a period of growth and innovation and the deeply challenging onset of the COVID-19 pandemic.
Oklahoma Health Care Authority Chooses UnitedHealthcare to Serve its Medicaid Beneficiaries
The Oklahoma Health Care Authority, which is partnering with managed care health plans to improve people’s health outcomes, increase access to care, and reduce health care costs, selected UnitedHealthcare Community Plan of Oklahoma to administer its statewide Medicaid program, SoonerSelect, starting later this year.
UnitedHealth Group Reports Fourth Quarter and Full Year 2020 Financial Results
Fundamental execution was strong across UnitedHealth Group (NYSE: UNH) in the fourth quarter and throughout the full year 2020, led by Optum and by UnitedHealthcare’s community and senior benefit businesses, even as the Company delivered expansive voluntary relief efforts for consumers, care providers and customers across the health system.
UnitedHealthcare Expands Access to Virtual Care, Including a New Virtual Primary Care Offering
UnitedHealthcare has expanded the availability of virtual care with local physicians for members enrolled in employer-sponsored plans, and also introduced a new Virtual Primary Care service designed to enable access to medical services in a simpler and more convenient way.
OptumInsight and Change Healthcare Combine to Advance a More Modern, Information and Technology-Enabled Health Care Platform
Optum, a diversified health services company and part of UnitedHealth Group, and Change Healthcare, a health care technology leader, have agreed to combine.
UnitedHealthcare Introduces Enhancements for Wearable Device Well-being Program, Including Access to Apple Fitness+ at No Additional Cost
UnitedHealthcare Motion, a wearable device well-being program available for purchase to employers across the country with self-funded and fully insured health plans, introduced several enhancements to eligible participants, which begin Jan. 1.
Optum Expands Partnership with Wider Circle to Deliver 25,000 Healthy Meals to Individuals and Families in Need during Holiday Season
Optum, a leading health services company, is expanding its partnership with Wider Circle, a tech-enabled community-based health care services company that drives better health for older adults and other vulnerable communities, to bring 25,000 meals to individuals and families, including Optum patients in Los Angeles County, during the holiday season.
Lilly and UnitedHealth Group partner on pragmatic study of neutralizing antibody bamlanivimab (LY-CoV555) for COVID-19
Eli Lilly and Company (NYSE: LLY) and UnitedHealth Group (NYSE: UNH) today announced a partnership to conduct a pragmatic study of bamlanivimab (LY-CoV555) in high-risk, COVID-19 infected individuals.
UnitedHealthcare Awards Nearly $100,000 in Community Builder Grants to Six Community Organizations in Michigan
Amid the ongoing COVID-19 pandemic UnitedHealthcare Community Plan of Michigan has awarded nearly $100,000 in Community Builder Grants to six community organizations aimed at improving access to health care services and addressing social determinants of health.
Sir Andrew Witty Returns to UnitedHealth Group after Leave of Absence
UnitedHealth Group (NYSE: UNH) announced that Sir Andrew Witty, president of UnitedHealth Group and chief executive officer of Optum, has returned to the company after an eight-month leave of absence to serve as a Global Envoy for the World Health Organization’s COVID-19 efforts.
UnitedHealth Group Updates Business Outlook Ahead of Investor Conference
UnitedHealth Group issued an updated 2020 outlook and its initial view of 2021 ahead of its annual Investor Conference.
UnitedHealth Group to Host 2020 Investor Conference
UnitedHealth Group will host its annual Investor Conference with analysts and institutional investors virtually on Tuesday, December 1, 2020, beginning at 9:00 a.m. ET.
UnitedHealth Group Names Matthew W. Friedrich Chief Legal Officer
UnitedHealth Group (NYSE: UNH) has named Matthew W. Friedrich executive vice president and chief legal officer, effective January 11, 2021.
United Health Foundation and Any Baby Can Partner to Expand Maternal Care for At-Risk Women in Texas
The United Health Foundation is teaming up with Any Baby Can (ABC) to expand at-home maternal care services and improve the health of at-risk prenatal women.
UnitedHealth Group Named to Dow Jones Sustainability North America and World Indices for 22nd Consecutive Year
Within the Health Care Equipment and Services Industry Group, UnitedHealth Group ranked in the 96th percentile overall, up 1 point from last year.
United Health Foundation and Texas Association of Community Health Centers Announce Partnership to Better Serve Adults Living with Diabetes
The United Health Foundation today announced a partnership with the Texas Association of Community Health Centers (TACHC) to provide better care for adults living with diabetes across the state of Texas.
UnitedHealth Group Board Authorizes Payment of Quarterly Dividend
The UnitedHealth Group (NYSE: UNH) board of directors has authorized payment of a cash dividend of $1.25 per share, to be paid on December 15, 2020, to all shareholders of record of UnitedHealth Group common stock as of the close of business on December 7, 2020.
More Than 40% of Americans Say COVID-19 Has Influenced What Health Plan They Intend to Select During Open Enrollment
Many Americans said COVID-19 has influenced the health plan they intend to select during open enrollment.
Confidence in Artificial Intelligence Increases as Health Industry Leaders Project Faster Return on Investment, Signal Growing Need for Broad Range of AI Expertise
Health care executives today believe artificial intelligence (AI) will deliver value for the industry faster than previously thought.
United Health Foundation Partners with Family First Health of Pennsylvania to Improve Access to Care for Children and Families
The United Health Foundation is partnering with Family First Health, a federally qualified health center, on an innovative program to improve access to health care for children and their families while widening the reach to serve vulnerable populations in the Keystone State.
New Partnership with University of California, San Francisco Will Help Grow and Diversify State’s Mental Health Workforce
A four-year, $4 million grant partnership between the University of California, San Francisco and UnitedHealth Group will expand the mental health workforce in California.
UnitedHealth Group and University of California San Diego Teaming to Help Grow and Diversify State’s Mental Health Workforce
The University of California San Diego and UnitedHealth Group are announcing a new four-year, $4 million grant collaboration to expand the mental health workforce in California.
United Health Foundation Pledges $2.5 Million to Support Breast Cancer Screenings for Michigan Residents
The United Health Foundation has committed $2.5 million to the Michigan Primary Care Association (MPCA) to support increased breast cancer screening and genetic testing for high-risk women, men and their families.
UnitedHealth Group Reports Third Quarter Results
During the third quarter of 2020, UnitedHealth Group (NYSE: UNH) saw continued growth, led by Optum and the UnitedHealthcare public-sector and senior benefits businesses, even as the Company continued its expansive COVID-19 response efforts supporting patients, care providers, customers and communities.
Sanvello Teams Up With the Chicago Bulls to Increase Access to Mental Health Resources for Youth
Sanvello Health, Inc., a leading digital mental health care provider and UnitedHealth Group company (NYSE:UNH), today announced a new partnership with the Chicago Bulls.
UnitedHealth Group Launches The HERO Program™ to Remove Financial Barriers for Living Donor Transplants
UnitedHealth Group (NYSE: UNH) has launched a first-of-its-kind program designed to support employees, and boost the critically low number of live-organ transplants.
UnitedHealthcare Eye Care Program Helps Support Children’s Eye Health by Reducing Exposure to Blue Light Amid COVID-19
UnitedHealthcare has launched a vision program that will help children across the country reduce their exposure to blue light and support their overall eye health, addressing the unique eye-health challenges young people may face amid COVID-19.
United Health Foundation and American Academy of Family Physicians Foundation Partner to Promote Physician Well-Being and Reduce Burnout
United Health Foundation is teaming with the American Academy of Family Physicians (AAFP) Foundation through a $3 million, three-year grant to help the AAFP identify causes of physician burnout and develop solutions to improve physician wellness and, ultimately, deliver higher quality care to patients.
UnitedHealthcare’s 2021 Medicare Plans Bring Unique Solutions for Unique Times
UnitedHealthcare® today introduced its 2021 Medicare Advantage and prescription drug plans, showcasing affordable coverage, exclusive benefits, expanded plan access and a simplified member experience that connects people to quality care – when and where they need it.
UnitedHealthcare Donates $1 Million to Support Food Security and Housing Programs Offered by Catholic Charities of Southern Nevada
UnitedHealthcare announced today it will contribute $1 million to Catholic Charities of Southern Nevada over the next three years to provide vital support to their Meals on Wheels program and Renewing Hope Program for Men.
UnitedHealthcare Introduces New Health Plan Offering Lower Premiums and a High-Performing Network in Kansas City
Kansas City-area employers can save up to 15% on monthly premiums with a new health plan from UnitedHealthcare that features Saint Luke’s Health System and Children’s Mercy Kansas City in its high-performing network.
United Health Foundation Partners with Florida State University to Establish Graduate-Level Concentration in Military Health
The United Health Foundation has committed $1.25 million to Florida State University (FSU) College of Nursing to help nurse practitioners better address the distinct health needs of individuals who have served in the U.S. Armed Forces.
UnitedHealthcare and Optum Take Action to Support People Affected by Ongoing Wildfires in Western States
We're taking action to help people affected by the ongoing wildfires across parts of California, Oregon, Washington and several other Western States.
UnitedHealthcare and Canopy Health Introduce Health Plan Delivering Lower Costs and a Patient-Focused Health Care Experience
UnitedHealthcare and Canopy Health have introduced a new health plan that offers consumers in Northern California personalized and seamless customer support as well as the opportunity to save up to 25% on premiums.
UnitedHealthcare and Sesame Workshop Team Up to Help Families Grow in Healthy Ways
UnitedHealthcare and Sesame Workshop, the nonprofit educational organization behind Sesame Street, are co-creating a webinar designed to keep grandparents and their grandchildren connected during COVID-19.
World-Champion Gymnast Aly Raisman Partners with Sanvello to Advance Mental Health Solutions
Sanvello Health, Inc., a leading digital mental health care provider and a UnitedHealth Group (NYSE: UNH) company, today announced a new partnership with gold medal gymnast and wellness advocate, Aly Raisman. The news strategic partnership also comes as Sanvello launches its new mental health coaching services and an expanded therapy offering, both available within the app.
UnitedHealthcare Donates $500,000 to Support Residents of Louisiana Affected by Hurricane Laura
UnitedHealthcare announced today it is donating $500,000 to the Community Foundation of Southwest Louisiana to help residents recover and rebuild following the devastating impact of Hurricane Laura.
State of Indiana Chooses UnitedHealthcare to Serve its Hoosier Care Connect Program Beneficiaries
The Indiana Family and Social Services Administration, which is partnering with managed care health plans to improve people’s health and well-being and reduce health care costs, has selected UnitedHealthcare to administer its Hoosier Care Connect program.
Morehouse School of Medicine and UnitedHealth Group Collaborate to Help Expand COVID-19 Research and Health Equity for Individuals with Sickle Cell
Morehouse School of Medicine (MSM) and UnitedHealth Group (NYSE: UNH) have joined forces to determine if people with sickle cell trait are at greater risk of contracting COVID-19 and if the trait results in more severe cases of the disease.
United Health Foundation Pledges $1.7 Million to Health Care Center for the Homeless to Expand Access to Primary Care in Florida
The United Health Foundation has committed $1.7 million to increase the number of health care providers by training nurse practitioners to meet growing demand for primary care in underserved communities of Florida.
United Health Foundation Donates $1,250,000 to ECU to Support Maternal Health Needs of North Carolina Amid COVID-19 Pandemic
The United Health Foundation has donated $1,250,000 to East Carolina University’s Brody School of Medicine to expand access to health care and improve health outcomes for North Carolina’s mothers and babies.
United Health Foundation Donates $750,000 to Support Maternal Health Needs of Georgia Amid COVID-19 Pandemic
The United Health Foundation has donated $750,000 to the Healthy Mothers, Healthy Babies Coalition of Georgia to improve access to health care and health outcomes for Georgia’s mothers and babies.
UnitedHealth Group Board Authorizes Payment of Quarterly Dividend
The UnitedHealth Group (NYSE: UNH) board of directors has authorized payment of a cash dividend of $1.25 per share, to be paid on September 22, 2020, to all shareholders of record of UnitedHealth Group common stock as of the close of business on September 14, 2020.
UnitedHealth Group Publishes Inaugural Sustainability Report
Annual report is a snapshot of the company’s efforts to lead in the development of the next-generation health system in a socially conscious way
UnitedHealthcare Donates More than $100,000 to Nonprofits in Arizona
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, is awarding $105,000 in Empowering Health grants to three community-based organizations in Arizona to expand access to care and address the social determinants of health for uninsured individuals and underserved communities.
UnitedHealth Group Continues Efforts to Combat Covid-19, Reports Second Quarter Performance
During the second quarter of 2020, UnitedHealth Group (NYSE: UNH) expanded its COVID-19 response efforts, proactively supporting patients, customers, care providers and communities.
Boulder Community Health and Optum Launch New, Comprehensive Relationship to Advance Quality Care and Improve Experiences for Patients in the Boulder Area
Boulder Community Health (BCH) and Optum today announced a comprehensive new relationship focused on advancing delivery of high-quality, convenient and affordable health care to patients across Boulder County and surrounding communities.
Innovative New Level2™ Digital Health Therapy Resulted in Better Health for People with Type 2 Diabetes
UnitedHealth Group (NYSE: UNH) has launched an innovative new therapy that combines wearable technology and customized personal support to help improve the health of people living with type 2 diabetes.
UnitedHealthcare Donates Nearly $1.1 Million to Nonprofits in Florida
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, is awarding nearly $1.1 million in Empowering Health grants to eight community-based organizations in Florida to expand access to care and address the social determinants of health for uninsured individuals and underserved communities.
UnitedHealthcare Donates $250,000 to Nonprofits Serving Charleston, West Virginia
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, is awarding $250,000 in Empowering Health grants to three community-based organizations in Charleston to expand access to care and address the social determinants of health for uninsured individuals and underserved communities.
UnitedHealthcare Donates More Than $1 Million to Nonprofits in Texas
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, is awarding more than $1 million in Empowering Health grants to eight community-based organizations in Texas to expand access to care and address the social determinants of health for uninsured individuals and underserved communities.
UnitedHealthcare Donates $1.3 Million to Nonprofits in New York
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, is awarding more than $1.3 million in Empowering Health grants to 14 community-based organizations in the state of New York to expand access to care and address the social determinants of health for uninsured individuals and underserved communities.
UnitedHealthcare Donates Nearly $1 Million to Nonprofits in South Carolina
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, is awarding nearly $1 million in Empowering Health grants to eight community-based organizations in South Carolina to expand access to care and address the social determinants of health for uninsured individuals and underserved communities.
UnitedHealthcare Donates Over $200,000 to Nonprofits in Pennsylvania
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, is awarding more than $207,000 in Empowering Health grants to three community-based organizations in Pennsylvania to expand access to care and address the social determinants of health for uninsured individuals and underserved communities.
UnitedHealthcare Donates $1 Million to Nonprofits in Nebraska
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, is awarding $1 million in Empowering Health grants to four community-based organizations in Nebraska to expand access to care and address the social determinants of health for uninsured individuals and underserved communities.
UnitedHealthcare Donates $1 Million to Nonprofits in Georgia
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, is awarding $1 million in Empowering Health grants to six community-based organizations in Georgia to expand access to care and address the social determinants of health for uninsured individuals and underserved communities.
UnitedHealthcare Donates Nearly $600,000 to Nonprofits in Tennessee
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, is awarding $595,000 in Empowering Health grants to six community-based organizations in Tennessee to expand access to care and address the social determinants of health for uninsured individuals and underserved communities.
UnitedHealthcare Donates $1 Million to Nonprofits in Kansas
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, is awarding $1 million in Empowering Health grants to seven community-based organizations in Kansas to expand access to care and address the social determinants of health for uninsured individuals and underserved communities.
UnitedHealthcare Donates $1 Million to Nonprofits in Maryland
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, is awarding $1 million in Empowering Health grants to eight community-based organizations in Maryland to expand access to care and address the social determinants of health for uninsured individuals and underserved communities.
UnitedHealthcare Donates $1 Million to Nonprofits in North Carolina
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, is awarding $1 million in Empowering Health grants to six community-based organizations in North Carolina to expand access to care and address the social determinants of health for uninsured individuals and underserved communities.
UnitedHealthcare Donates Nearly $600,000 to Nonprofits in Ohio
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, is awarding $595,000 in Empowering Health grants to seven community-based organizations in Ohio to expand access to care and address the social determinants of health for uninsured individuals and underserved communities.
Urgent Care Centers Can Address Gaps in Access to Primary Care According to New Research from UnitedHealth Group
New research from UnitedHealth Group has shown that urgent care centers can serve up to 10 million American children who currently have limited access to well-child visits.
UnitedHealthcare Dental Launches Teledentistry Option to Help Plan Participants Avoid Unnecessary ER Visits
UnitedHealthcare Dental continues to evolve its products and services to improve access to oral care, while lowering costs.
United Health Foundation Pledges $500,000 to Support Vulnerable Arizona Residents Amid COVID-19 Emergency
The United Health Foundation has committed $500,000 to provide urgent assistance to Arizona residents during the COVID-19 pandemic.
United Health Foundation Grants $430K to American Indian College Fund to Expand Tribal Scholars Program
The United Health Foundation (UHF) is increasing its support of the American Indian College Fund’s United Health Foundation Tribal Scholars Program to ensure Native American communities have access to urgently needed health care with a $430,000 grant to provide 13 scholarships for American Indian and Alaska Natives studying in the health and dental fields.
UnitedHealth Group Recognized by Points of Light as One of the 50 Most Community-Minded Companies in the United States
UnitedHealth Group (NYSE: UNH) has been recognized by The Civic 50 as one of the 50 most community-minded companies in the United States for its civic engagement in 2019.
Commonwealth of Kentucky Chooses UnitedHealthcare to Serve its Medicaid Beneficiaries
The Commonwealth of Kentucky, which is partnering with managed care health plans to improve people’s health and well-being and reduce health care costs, selected UnitedHealthcare Community Plan of Kentucky as one of five organizations to administer its statewide Medicaid program, effective January 1, 2021.
UnitedHealth Group Invests Additional $100 Million in Affordable Housing to Further Its Commitment to Building Communities That Achieve Better Health Outcomes
UnitedHealth Group (NYSE: UNH) has reached $500 million in affordable housing investments, with an announcement today of a $100 million investment in the Health & Housing Fund — a partnership with Stewards of Affordable Housing for the Future (SAHF) and National Affordable Housing Trust (NAHT).
UnitedHealth Group Updates on Annual Shareholder Meeting, Board Actions
UnitedHealth Group (NYSE: UNH) provided updates on its 2020 annual shareholder meeting and actions by its Board of Directors at its regular quarterly meeting.
UnitedHealth Group Announces Support for Twin Cities in Response to George Floyd Tragedy and Civil Unrest
Following the tragic death of George Floyd, UnitedHealth Group (NYSE: UNH) today announced a commitment to support Mr. Floyd’s family, help Twin Cities businesses restore their operations and fund efforts to advance equity and inclusivity in the Minneapolis-St. Paul community.
United Health Foundation Commits $2.5 Million to Establish Behavioral Health Crisis Team in Children’s Wisconsin Emergency Department
The United Health Foundation has awarded Children’s Wisconsin a three-year, $2.5 million grant to establish a crisis response team in the emergency department (ED) available 24 hours a day, seven days a week for children with mental and behavioral health needs.
Rally Health Earns HITRUST CSF Certification for Meeting Regulatory and Industry-Defined Requirements for Safeguarding Protected Health Information
Digital health company Rally Health, Inc., part of health services leader Optum, announced today that its Rally® consumer digital health platform and entire portfolio of solutions have achieved HITRUST CSF® Certification, a distinction awarded by HITRUST,® a leading data protection standards development and certification organization, to recognize health solutions that have passed a rigorous security evaluation and have met key regulations and industry requirements related to safeguarding protected health information (PHI).
Study Finds Seniors with COVID-19 Taking Hypertension Medication at Lower Risk of Hospitalization, Clinical Trial to Follow Immediately
A study completed by UnitedHealth Group (NYSE: UNH) with the Yale School of Medicine found that older COVID-19 patients with hypertension taking angiotensin-converting enzyme (ACE) inhibitors had a lower risk of COVID-19 hospitalization.
UnitedHealth Group-Sponsored Charity Golf Match Raises Millions for American Nurses Foundation and CDC Foundation to Support COVID-19 Response
The TaylorMade Driving Relief charity golf match, supported by UnitedHealth Group (NYSE: UNH), raised more than $5.5 million for COVID-19 relief efforts, led by UnitedHealth Group’s $3 million contribution to benefit the American Nurses Foundation and CDC Foundation, two organizations helping to lead COVID-19 relief efforts.
UnitedHealth Group and Microsoft Collaborate to Launch ProtectWell Protocol and App to Support Return-to-Workplace Planning and COVID-19 Symptom Screening
UnitedHealth Group and Microsoft Corp. have joined forces to launch ProtectWell, an innovative return-to-workplace protocol that enables employers to bring employees back to work in a safer environment.
UnitedHealthcare Community Plan of Ohio Awarded NCQA Distinction in Multicultural Health Care
The National Committee for Quality Assurance (NCQA) has recognized UnitedHealthcare Community Plan of Ohio with its Distinction in Multicultural Health Care award for delivery of culturally appropriate and quality improvement interventions serving diverse populations.
UnitedHealthcare and GlassesUSA.com’s New Network Relationship Gives People Online Access to Affordable, Designer Prescription Eyewear
People enrolled in UnitedHealthcare employer-sponsored and individual vision plans now have network access to GlassesUSA.com, giving more than 19 million Americans online access to order prescription glasses and sunglasses for little or no out-of-pocket costs.
United Health Foundation Donates $750,000 to Support Pennsylvania’s Home Care, Home Health and Hospice Workers Amid COVID-19 Emergency
The United Health Foundation has donated $750,000 to provide personal protective equipment (PPE) and support for frontline health care workers fighting COVID-19 and the vulnerable populations they serve in Pennsylvania.
Optum Offers Free Online Wellness Program to Help Older Adults Stay Healthy and Active During COVID-19 Pandemic
Optum, a leading health services company, launched the Virtual Community Center wellness program to give older adults across the country free access to online exercise, nutrition and mental health classes geared for their age group.
Optum Helping People Stay Connected with Needed Behavioral Health Support During COVID-19
Optum continues to respond to the need by significantly expanding the availability of telehealth visits, including growing the number of providers available to see patients virtually.
UnitedHealth Group Provides Over $1.5 Billion of Additional Support in Response to Covid-19 Challenges
UnitedHealth Group (NYSE: UNH) is taking additional action to directly support people affected by the COVID-19 pandemic by providing over $1.5 billion of additional support for its customers.
United Health Foundation Donates $500,000 to Support Behavioral Health Needs of Colorado Residents Amid COVID-19 Emergency
The United Health Foundation has donated $500,000 to the Colorado Community Health Network (CCHN) to address the behavioral health needs of Colorado residents during the COVID-19 pandemic.
United Health Foundation Donates $500,000 to University of Chicago Medicine to Support Expanded COVID-19 Testing in Underserved Communities
The United Health Foundation is donating $500,000 to the University of Chicago Medicine to support expanded COVID-19 testing for underserved communities.
UnitedHealth Group, Boston Scientific, Medtronic and the University of Minnesota Work to Deploy 3,000 Emergency Ventilator Alternative Devices
UnitedHealth Group is collaborating with Boston Scientific, Medtronic and the University of Minnesota to deploy 3,000 newly invented “light” ventilators to address the limited stock of critical breathing support equipment in response to COVID-19.
United Health Foundation Joins Forces with AARP Foundation in $5 Million Initiative to Support Seniors Experiencing Isolation, Food Insecurity, During COVID-19 Crisis
The United Health Foundation is teaming up with AARP Foundation to support older Americans during the COVID-19 emergency.
UnitedHealth Group Donates $5 Million to Support National Program to Develop Convalescent Plasma Treatments for COVID-19
UnitedHealth Group (NYSE: UNH) will donate $5 million to support a federally sponsored program aimed at accelerating and expanding the availability of investigational convalescent plasma treatments for COVID-19 patients nationwide.
United Health Foundation Launches $5 Million in National Partnerships to Support Frontline Health Care Workers During COVID-19 Emergency
The United Health Foundation is partnering with the CDC Foundation, Direct Relief and the American Nurses Foundation to support the nation’s health care workforce during the COVID-19 crisis.
New Study Shows Effectiveness of Polyester Swabs and Saline Transportation for COVID-19 Testing, Improving Testing Efficiency and Flexibility, and Protecting Health Care Workers
A study led by UnitedHealth Group (NYSE: UNH) Research & Development and The Everett Clinic, part of Optum, revealed alternative swab materials and commonly available saline are effective for COVID-19 testing, providing more options for sample collection.
Sanvello Offers Free Clinician Dashboard to Mental Health Professionals to Support COVID-19 Response
Sanvello Health, Inc., a leading provider of digital and tele-mental health solutions to individuals, businesses and health care professionals, today announced free access to its clinician dashboard, Sanvello for Clinicians, to all U.S. mental health professionals to support their work with patients during the COVID-19 pandemic for the duration of the crisis.
UnitedHealth Group Reports First Quarter Results
During the first quarter of 2020, UnitedHealth Group (NYSE: UNH) responded to the COVID-19 global health crisis, rapidly redirecting its business efforts to provide a broad range of critical support to patients, customers, care providers and communities, while maintaining full employment for its team members.
Sir Andrew Witty to Take Leave of Absence from UnitedHealth Group to Co-Lead World Health Organization Efforts to Accelerate a COVID-19 Vaccine
UnitedHealth Group (NYSE: UNH) announced that Sir Andrew Witty, president of UnitedHealth Group and CEO of Optum, has been asked to co-lead a global effort of the World Health Organization (WHO), in partnership with key stakeholders, to accelerate the development of a COVID-19 vaccine.
United Health Foundation Pledges $250,000 to Support Vulnerable Michigan Residents Amid COVID-19 Emergency
The United Health Foundation has committed $250,000 to provide urgent assistance to Michigan residents experiencing food insecurity as they face unprecedented hardships during the COVID-19 pandemic.
United Health Foundation Pledges $1 Million to Support Vulnerable Los Angeles County Residents Amid COVID-19 Emergency
The United Health Foundation has committed $1 million to provide urgent assistance to Los Angeles County residents experiencing homelessness as they face unprecedented hardships during the COVID-19 pandemic.
UnitedHealth Group Honored to Assist the U.S. Department of Health and Human Services Under the CARES Act
UnitedHealth Group is honored to have been asked to assist the U.S. Department of Health and Human Services in distributing, as directed by the Department, an initial $30 billion in emergency funding to health care providers seeking assistance under the CARES Act. This effort is vital to maintaining the health and readiness of the U.S. health care system, and we’re pleased to have the opportunity to support it.
United Health Foundation Pledges $1 Million to Support Vulnerable New York Residents Amid COVID-19 Emergency
Partnerships with Food Bank For New York City and Care For the Homeless are part of initial $50 million commitment from UnitedHealth Group to fight COVID-19 and support impacted communities
United Health Foundation Pledges $500,000 to Support Vulnerable Louisiana Residents Amid COVID-19 Emergency
The United Health Foundation has committed $500,000 to provide urgent assistance to Louisiana residents experiencing homelessness and food insecurity as they face unprecedented hardships during the COVID-19 pandemic.
United Health Foundation Pledges $1 Million to Support Vulnerable New Jersey Residents Amid COVID-19 Emergency
The United Health Foundation has committed $1 million to provide urgent assistance to New Jersey residents experiencing food insecurity as they face unprecedented hardships during the COVID-19 pandemic.
UnitedHealth Group Commits Additional $10 Million for COVID-19 International Response
UnitedHealth Group (NYSE: UNH) will contribute an initial $10 million to fight the COVID-19 pandemic internationally in countries where its UnitedHealthcare and Optum businesses operate, including in Brazil, Chile, Colombia, India, Ireland, Peru, Philippines and Portugal.
United Health Foundation Pledges $1 Million to Support Vulnerable Seattle Residents Amid COVID-19 Emergency
The United Health Foundation has committed $1 million to provide urgent assistance to Seattle residents experiencing homelessness as they face unprecedented hardships during the COVID-19 pandemic.
United Health Foundation Pledges $1 Million to Support Vulnerable Florida Residents Amid COVID-19 Emergency
The United Health Foundation has committed $1 million to provide urgent assistance to Florida residents experiencing homelessness and food insecurity as they face unprecedented hardships during the COVID-19 pandemic.
UnitedHealthcare, Optum Turn Cafeteria Into Meal-Prep Base for Hartford Residents in Need
UnitedHealthcare of New England and Optum reallocate their campus cafeteria staff to provide up to 11,200 meals each week, at least for the next seven weeks.

UnitedHealth Group Accelerates Nearly $2 Billion in Payments and Support to Health Care Providers to Help with COVID-19 Financial Challenges
UnitedHealth Group, through UnitedHealthcare and Optum, has announced it is taking steps immediately to accelerate payments and other financial support to health care providers in the U.S. to help address the short-term financial pressure caused by the COVID-19 emergency.
Health Plan of Nevada and Southwest Medical Associates Turn Headquarters Cafeteria into Meal Prep Base for Those in Need
Thousands of Las Vegas area homeless will have access to healthy meals, as UnitedHealth Group’s Southern Nevada-based companies reallocate their campus cafeteria staff to provide 10,500 meals each week
United Health Foundation Supports Americans Experiencing Homelessness and Food Insecurity Amid COVID-19 Emergency
The United Health Foundation has pledged $5 million to provide urgent support for people experiencing homelessness and food insecurity as they face unprecedented hardships during the COVID-19 pandemic.
UnitedHealth Group Leads Meal-Prep Effort for Twin Cities Residents in Need
Thousands of Twin Cities families will have access to free and healthy food, as UnitedHealth Group (NYSE: UNH) leads an effort to create and provide 21,000 meals each week, for the next eight-plus weeks.
UnitedHealth Group Commits Initial $50 Million to Combat COVID-19 and Support Affected Communities
UnitedHealth Group Study Clears Path for Self-Administered COVID-19 Test, Improving Testing Efficiency and Protecting Health Care Workers
A study led by UnitedHealth Group (NYSE: UNH) Research & Development and OptumCare clinicians has demonstrated that a simple, self- collected test is as effective in identifying COVID-19 infections as the current clinician-collected test.
UnitedHealthcare Offers Special Enrollment and Reduces Administrative Requirements to Improve Access to Care and Coverage in Response to COVID-19
UnitedHealthcare announced today several updates to its programs in response to the COVID-19 national emergency.
Sanvello Offers Free Premium Access to Help People Cope With Mental Health Impacts of COVID-19
Sanvello Health, Inc., a leading provider of digital and tele-mental health solutions to individuals, businesses and payers, today announced free premium access to its digital care delivery platform.
UnitedHealthcare Expands Access to Care, Support and Resources to Help People and Families Address COVID-19
UnitedHealthcare announced today several updates that provide people and families expanded access to the care, support and resources they need to navigate through this unprecedented time.
New UnitedHealthcare Eye Care Benefit Gives Expectant and New Moms Improved Access to Comprehensive Eye Exams and Glasses
UnitedHealthcare has introduced a new benefit program to support the eye health and overall well-being of expectant and new moms, helping expand access to recommended vision care before and after delivery.
UnitedHealth Group Reinforces Actions Taken to Provide Members and Patients with COVID-19 Support and Resources
UnitedHealth Group (NYSE: UNH), UnitedHealthcare and Optum are taking action to ensure health plan members and patients affected by COVID-19 have the support and resources they need.
UnitedHealth Group Donates $150,000 to Help Residents of Tennessee Affected by Tornadoes and Severe Weather
UnitedHealth Group (NYSE: UNH) and its UnitedHealthcare and Optum businesses are donating $150,000 to help residents of Tennessee recover and rebuild from the tornadoes and severe weather around Nashville.
UnitedHealthcare Helps Confront the Opioid Epidemic with New Oral Health Public Toolkit
UnitedHealthcare has expanded its efforts to help address the connection between dental care and the opioid epidemic, introducing a public toolkit with information to help support oral health care professionals and patients, especially after wisdom-teeth removal for teens and young adults.
UnitedHealthcare and Optum Take Action to Support People Affected by Floods in Mississippi
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people who may be affected by the recent floods in Mississippi.
UnitedHealth Group Board Authorizes Payment of Quarterly Dividend
The UnitedHealth Group (NYSE: UNH) board of directors has authorized payment of a cash dividend of $1.08 per share, to be paid on March 24, 2020, to all shareholders of record of UnitedHealth Group common stock as of the close of business on March 16, 2020.
UnitedHealthcare and Optum Take Action to Support People Affected by Severe Weather in Mississippi
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people who may be affected by the severe weather in Mississippi.
UnitedHealth Group Reports 2019 Results
Diversified strength in performance continued across UnitedHealth Group (NYSE: UNH) in the fourth quarter and full year 2019.
UnitedHealthcare and Optum Take Action to Support People Affected by Earthquakes in Puerto Rico
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people who may be affected by the recent earthquakes in Puerto Rico.
Genoa Healthcare Opens 500th Pharmacy Serving Behavioral Health Patients
Genoa Healthcare, a leading provider of behavioral pharmacy and medication management services, has opened its 500th pharmacy in the United States serving patients with mental health, substance use disorders and other complex, chronic health conditions.
Diplomat, OptumRx Combining to Advance Access to Specialty Pharmacy Care and Infusion Services, Improve Health Outcomes
OptumRx, the pharmacy care services business of Optum, and Diplomat, a provider of specialty pharmacy and infusion services, are combining.
America’s Health Rankings 2019 Annual Report Marks 30 Years of Public Health Progress and Challenges
Today, the United Health Foundation released the 2019 America’s Health Rankings® Annual Report, which highlights health trends from the past three decades as well as from the past year.
UnitedHealth Group to Discuss Business Outlook at Investor Conference
UnitedHealth Group (NYSE: UNH) will host its annual Investor Conference with analysts and institutional investors in New York City on Tuesday, December 3, 2019, beginning at 8:00 a.m. EST.
UnitedHealthcare to Open Member Medicare Services Centers in Select Walgreens Stores
UnitedHealthcare®, the health benefits business of UnitedHealth Group (NYSE: UNH), and Walgreens will open 14 UnitedHealthcare Medicare services centers within Walgreens stores in five metropolitan areas as part of a multiyear agreement.

United Health Foundation and the Colorado Center for Nursing Excellence Partner to Increase Access to Behavioral Health Care Services for Residents of Rural Colorado
The United Health Foundation is partnering with the Colorado Center for Nursing Excellence (the Center) to address the shortage of mental health providers in rural Colorado communities.
UnitedHealth Group to Host Investor Conference
UnitedHealth Group (NYSE: UNH) will host its annual Investor Conference with analysts and institutional investors in New York City on Tuesday, December 3, 2019, beginning at 8:00 a.m. EST.
Sir Andrew Witty Named UnitedHealth Group President
UnitedHealth Group (NYSE: UNH) has appointed Andrew Witty UnitedHealth Group President.
UnitedHealth Group Board Authorizes Payment of Quarterly Dividend
The UnitedHealth Group (NYSE: UNH) board of directors has authorized payment of a cash dividend of $1.08 per share, to be paid on December 17, 2019, to all shareholders of record of UnitedHealth Group common stock as of the close of business on December 9, 2019.
New UnitedHealthcare Benefit for Low Back Pain Helps Reduce Invasive Procedures and Address the Opioid Epidemic
UnitedHealthcare has introduced a new benefit for people with acute low back pain that makes it more affordable to access physical therapy and chiropractic care, helping to improve health outcomes, reduce costs and avoid often unnecessary invasive treatments and opioid prescriptions.
UnitedHealthcare and Optum Take Action to Support People Affected by Wildfires Across Parts of California
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people who may be affected by wildfires affecting parts of California.
UnitedHealthcare and Optum Take Action to Support People Affected by Severe Weather, Tornadoes in Dallas Area
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people who may be affected by severe weather, including tornadoes that struck parts of Dallas and the surrounding area.

United Health Foundation Partners with Morehouse School of Medicine to Expand Access to Digital Health Technologies for Rural and Underserved Communities
The United Health Foundation on Thursday announced a new partnership with the Morehouse School of Medicine’s National Center for Primary Care to examine how digital tools could be leveraged to support underserved and rural communities in four Southeastern states.
UnitedHealth Group Reports Third Quarter Results
Strong and diversified performance continued across UnitedHealth Group (NYSE: UNH) in the third quarter 2019.
New UnitedHealthcare App Now Gives Millions of Plan Participants On-Demand Access to Virtual Visits
Millions of Americans now have access to on-demand telemedicine services 24/7 with the new UnitedHealthcare app.
Artificial Intelligence Adoption and Investments Growing Rapidly Among Health Industry Leaders
Confidence and investment in artificial intelligence (AI) to improve health care remain high, according to a new survey of 500 U.S. health industry leaders from hospitals, health plans, life sciences and employers, on their attitudes and adoption of the technology.
UnitedHealthcare’s 2020 Medicare Plans Offer More Ways to Help People Stay Healthy and Save Money
UnitedHealthcare® today introduced its 2020 Medicare Advantage and prescription drug plans, providing people more value for their Medicare dollar.
Survey: More Americans Turn to Technology for Health Information, with a Record Number Now Comparison Shopping for Care
Many Americans want technology – such as artificial intelligence – to help make health care decisions, and a record number say they have used the internet and mobile apps to comparison shop for care, according to a new UnitedHealthcare survey.
UnitedHealthcare and Optum Take Action to Support People Affected by Severe Weather in Puerto Rico and the U.S. Virgin Islands
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people who may be affected by severe weather across parts of Puerto Rico and the U.S. Virgin Islands.
UnitedHealthcare and Optum Take Action to Support People in Texas Affected by Floods
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people who may be affected by severe weather and flooding across parts of Texas.
UnitedHealthcare to Offer New Medicare Advantage Plan Featuring Canopy Health Care Providers
UnitedHealthcare will offer a new Medicare Advantage plan in the Bay Area featuring Canopy Health care providers. The UnitedHealthcare® Canopy Health Medicare Advantage plan will be available to more than 630,000 Medicare beneficiaries in Contra Costa, Alameda and San Francisco counties.
America’s Health Rankings Health of Women and Children Report Shows Nationwide Increase in Teen Suicide and Child Mortality
Teen suicide and child mortality rates have increased sharply since the 2016 Report, according to the United Health Foundation’s 2019 America’s Health Rankings® Health of Women and Children Report.
UnitedHealth Group Named to Dow Jones Sustainability North America and World Indices for 21st Consecutive Year
UnitedHealth Group (NYSE: UNH) has been named to the Dow Jones Sustainability North America Index (DJSI NA) and the Dow Jones Sustainability World Index (DJSI W) for 2019 in the Health Care Equipment & Services Sector. This marks 21 consecutive years the company has been named to the indices, beginning in 1999 when the rankings were established.
Top Health and Aging Organizations Kick Off National Medicare Education Week with Free Events and Resources to Help Simplify Medicare Enrollment
To help simplify the process of learning about Medicare, Medicare beneficiaries, their families and caregivers are invited to attend free Medicare events and online webinars during National Medicare Education Week, Sept. 15-21, 2019.
UnitedHealthcare and Optum Take Action to Support People in Carolinas and Georgia Preparing for Hurricane Dorian
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people in the Carolinas and Georgia who may be affected by Hurricane Dorian. This is in addition to actions taken earlier to support individuals in Florida.
United Health Foundation and The Health Wagon Announce $1 Million Multiyear Partnership to Expand Access to Quality Care in Southwest Virginia
The United Health Foundation and The Health Wagon today announced a new partnership to expand access to vital health care services for thousands of people in communities throughout southwest Virginia.
UnitedHealthcare and Optum Take Action to Support People Affected by Severe Weather in Puerto Rico
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people affected by Tropical Storm Dorian across parts of Puerto Rico.
UnitedHealthcare and Optum Take Action to Support People Preparing for Severe Weather in Florida
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people who may be affected by Tropical Storm Dorian, which is expected to make landfall later this week.
UnitedHealthcare and Optum Take Action to Support People Affected by Wildfires in Alaska
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people affected by the ongoing wildfires across parts of Alaska.
UnitedHealthcare and Optum Take Action to Support People Affected by Severe Weather in Iowa
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people affected by severe weather in Madison, Marion and Warren counties in Iowa.
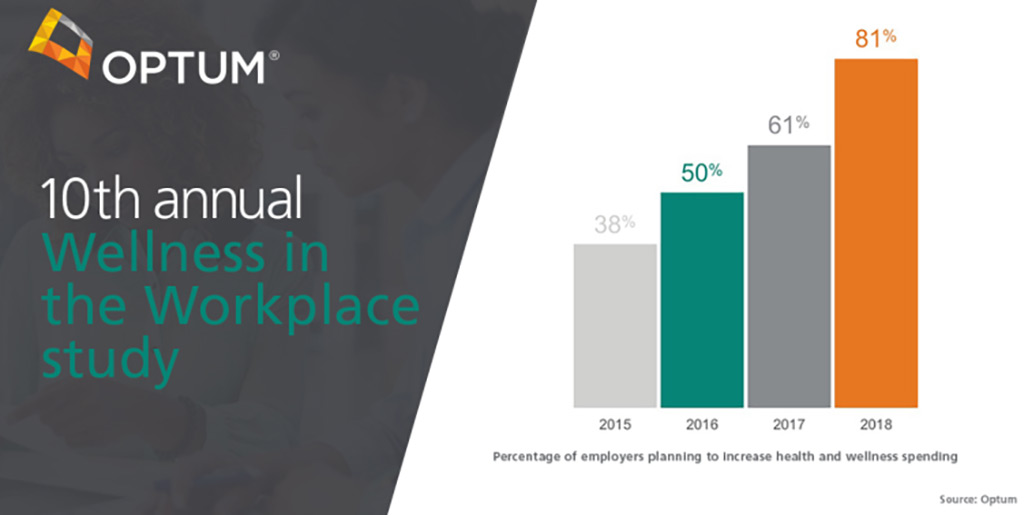
More than Twice as Many Employers than 10 Years Ago are Planning to Increase Investments in Employee Health and Wellness, Optum Study Shows
More than 80% of employers said they are planning to increase their health and wellness budgets this year, more than double compared to 2009 (34%), according to the 10th annual Optum Wellness in the Workplace study.
UnitedHealth Group Board Authorizes Payment of Quarterly Dividend to Shareholders
The Board of Directors of UnitedHealth Group (NYSE: UNH), at its regularly scheduled meeting, authorized payment of a cash dividend of $1.08 per share, to be paid on September 24, 2019, to all shareholders of record of UnitedHealth Group common stock as of the close of business on September 16, 2019.
Thousands of Optum Employee Volunteers Partner with Local Nonprofits in Five Countries to Help Reduce Health Disparities During Annual Day of Giving
Optum employee volunteers in the United States and around the world worked to make a difference in local communities where they work and live.
UnitedHealthcare to Continue to Serve Louisianans Enrolled in Medicaid
The Louisiana Department of Health selected UnitedHealthcare Community Plan to continue administering its Louisiana Medicaid program, effective Jan. 1, 2020.
UnitedHealth Group Supporting People Affected by Mass Shooting in El Paso
UnitedHealthcare and Optum, the health benefits and services businesses of UnitedHealth Group (NYSE: UNH), are opening Optum’s Emotional-Support Help Line, providing access to specially trained mental health specialists to support people affected by the recent mass shooting in El Paso.
UnitedHealth Group Supporting People Affected by Mass Shooting in Dayton
UnitedHealthcare and Optum, the health benefits and services businesses of UnitedHealth Group (NYSE: UNH), are opening Optum’s Emotional-Support Help Line, providing access to specially trained mental health specialists to support people affected by the recent mass shooting in Dayton.
UnitedHealthcare Awarding $1.1 Million to Northeast Ohio Nonprofits to Help Address Social Determinants of Health
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, is awarding $1.1 million in grants to four statewide and Cleveland-area community-based organizations to expand their services that address key social determinants of health, and improve care access and health outcomes.
UnitedHealth Group Reports Second Quarter 2019 Results
UnitedHealth Group (NYSE: UNH) reported second quarter 2019 results with continued well diversified strength in performance.
John Muir Health and Optum Launch New, Comprehensive Relationship to Advance Quality Care and Experiences for Patients in Bay Area
John Muir Health and Optum today announced a comprehensive new relationship focused on advancing delivery of high-quality, convenient and affordable health care to patients in the Bay Area. Optum brings an extensive set of capabilities to this innovative partnership, including operational technologies, analytic solutions and tools, and administrative services expertise to help John Muir Health further advance its clinical and operational performance.
UnitedHealthcare and Optum Take Action to Support People Affected by Tropical Storm Barry in Gulf States
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people who may be affected by severe weather and flooding across parts of Louisiana, Texas and Mississippi as a result of Tropical Storm Barry.

Helen Ross McNabb Center, University of Tennessee Medical Center and the United Health Foundation to Expand Access to Substance Abuse Treatment Services in Eastern Tennessee
To help thousands of Tennesseans and their families fight substance abuse and addiction, Helen Ross McNabb Center, The University of Tennessee Medical Center and the United Health Foundation are partnering to expand access to care providers and behavioral health services throughout East Tennessee.
UnitedHealthcare and Optum Take Action to Support People Affected by Recent Earthquakes in California
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people affected by the recent earthquakes and ensuing aftershocks across parts of California.
UnitedHealth Group Announces Atlanta HBCU Partnership, $8.25 Million Investment in the Education of Future Data Scientists
UnitedHealth Group and the Atlanta University Center Consortium (AUCC), the oldest and largest consortium of historically black colleges and universities (HBCUs), are partnering on a new initiative to prepare students to meet the growing demand in the marketplace for data analytics experts.
UnitedHealthcare and Optum Take Action to Support People Affected by Severe Weather and Flooding in West Virginia
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people affected by severe weather and flooding across parts of West Virginia.
UnitedHealthcare Awards Goodwill Industries of Kentucky $90,000 to Benefit Workforce Re-entry Program
UnitedHealthcare Community Plan of Kentucky awarded Goodwill Industries of Kentucky (Goodwill Kentucky) a $90,000 grant to help support people eligible for Medicaid, including those in the justice system who are re-entering society, with resources to find and sustain employment.
UnitedHealth Group Advances Senior Leadership Team
UnitedHealth Group (NYSE: UNH) announced changes to its senior executive team as part of its longstanding approach to building broad and deeply experienced leaders.
UnitedHealthcare and Optum Take Action to Support People Affected by Severe Weather and Flooding in Texas
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people affected by severe weather and flooding across parts of the Rio Grande Valley in Texas.
Launch of UnitedHealthcare Hearing Offers People Improved Access to Affordable, Quality Hearing Health Care
UnitedHealthcare has launched UnitedHealthcare Hearing, offering all consumers, including people enrolled in the company’s individual, employer-sponsored and Medicare Advantage plans, greater access to affordable, quality hearing health.
Older Americans Seek Meaning and New Experiences in Retirement Years; Say Health Is the Biggest Factor to Achieving Their Goals
In a new survey, nearly 70% of Americans ages 62 and older said physical health is most important to them as they age, followed in order by cognitive health (16%), social health (13%) and financial health (6%).
Optum completes acquisition of DaVita Medical Group from DaVita
Optum, a leading health services company, completed its acquisition of DaVita Medical Group, one of the nation’s leading independent medical groups, from DaVita Inc.
UnitedHealthcare Community Plan of Tennessee Awarded NCQA Distinctions
The National Committee for Quality Assurance (NCQA) has recognized UnitedHealthcare Community Plan of Tennessee with two awards – Distinction in Multicultural Health Care and Distinction in Long-Term Services and Supports (LTSS).
UnitedHealth Group Board Increases Shareholder Dividend
The Board of Directors of UnitedHealth Group (NYSE: UNH) authorized payment of a cash dividend of $1.08 per share, to be paid on June 25, 2019, to all shareholders of record of UnitedHealth Group common stock as of the close of business on June 17, 2019.
UnitedHealth Group Announces Results of 2019 Annual Shareholder Meeting
The Board of Directors of UnitedHealth Group (NYSE: UNH) announced the results of shareholder voting that took place during the Company’s 2019 annual meeting earlier today.
UnitedHealthcare and Optum Take Action to Support People Affected by Severe Weather and Flooding in Arkansas
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people affected by recent severe weather and flooding across parts of Arkansas.
Study: Many Americans Say They Are More Likely to Participate in a Fitness Routine if Given Opportunity to Socialize, Earn Financial Incentives
More than two-thirds of Americans say an incentive of as little as $2 per day would motivate them to devote at least an hour each day toward improving their health, while nearly 60 percent of people say they would be more likely to participate in a fitness routine if the program offered an opportunity to socialize or make friends, according to a new nationwide survey.
UnitedHealthcare and Optum Take Action to Support People Affected by Severe Weather and Flooding in Kansas
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people affected by recent severe weather and flooding across parts of Kansas.
UnitedHealthcare and Optum Take Action to Support People Affected by Severe Weather and Flooding in Oklahoma
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people affected by recent severe weather and flooding across parts of Oklahoma.
UnitedHealthcare Helps Make it Easier for People to Stay Fit and Save Money with Gym Check-In
UnitedHealthcare’s gym reimbursement program, Gym Check-In, has expanded to include more than 124,000 facilities across the United States, potentially saving consumers hundreds of dollars a year on their gym fees.
UnitedHealthcare and Optum Take Action to Support People Affected by Flooding in Missouri
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people affected by recent flooding across parts of Missouri.
UnitedHealthcare Community Plan Donates Drug Disposal Kits to Local Community Groups to Help People Safely Dispose of Unused Opioids
UnitedHealthcare Community Plan is confronting the opioid epidemic by donating 2,000 opioid disposal kits to the Byrnes Health Education Center and the Mural Arts Philadelphia’s Porch Light Program.
UnitedHealthcare Awards $1 Million Grant to Jordan Valley Community Health Center to Expand Use of Community Health Workers
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, has awarded a $1 million grant to Jordan Valley Community Health Center (JVCHC) to help the nonprofit expand its community health worker program.

Rally UHC Cycling Races "Inspired Bicycles" at Amgen Tour of California to Benefit UnitedHealthcare Children's Foundation
At the 2019 Amgen Tour of California, the Rally UHC Cycling team will once again ride six “Inspired Bikes” to benefit the UnitedHealthcare Children’s Foundation (UHCCF).

Increases in Home-Based Health Services Provide More Care Options for Seniors, According to New Report
Data released by the United Health Foundation’s 2019 America’s Health Rankings® Senior Report reveal there are 550,000 more home health care workers than last year – a 21 percent rate increase per 1,000 adults age 75 and older.
UnitedHealthcare and Optum Take Action to Support People Affected by Flooding in Mississippi
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people affected by flooding across parts of Mississippi.

UnitedHealthcare Awarding $1 Million to Memphis-Area Nonprofits to Help Address Social Determinants of Health
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, is awarding $1 million in grants to seven Memphis-area nonprofit organizations to expand their services that address key social determinants of health, and improve care access and patient outcomes.
UnitedHealthcare and Optum Take Action to Support People Affected by Flooding in Louisiana
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people affected by recent flooding across parts of Louisiana.
UnitedHealthcare Helps Support Moms’ and Babies’ Health Before and After Delivery with New Bundled Payment Program for Maternity Care
UnitedHealthcare, a UnitedHealth Group (NYSE: UNH) company, has introduced a new bundled payment program for maternity care to help support the well-being of moms and babies before and after delivery by closing gaps in care and encouraging healthy, full-term pregnancies.
HealthTrust Selects OptumRx as Exclusive Pharmacy Care Services Partner
HealthTrust, a leading group purchasing organization and health care performance improvement company, has selected OptumRx as its exclusive pharmacy care services partner for its member organizations.

Step up for Health and Step up for Kids – Participate in the 3rd Annual UHCCF Steppin’ Up for Kids Walk May 6-June 15
The UnitedHealthcare Children’s Foundation (UHCCF) is hosting the 3rd annual Steppin’ Up for Kids (SUFK) walk, a national initiative that encourages people to engage in healthier lifestyles on their own time while raising funds for medical grants for kids.

Smile Direct Club and UnitedHealthcare Help People Improve Their Smiles and Save Money
People enrolled in most UnitedHealthcare employer-sponsored and individual dental plans with orthodontic coverage can now purchase SmileDirectClub’s clear aligners for in most cases less than $1,000 out of pocket, helping plan participants improve their smiles, and potentially save time and thousands of dollars on orthodontic care.
UnitedHealthcare Focuses on Connecting Eligible Hawaii Medicare and Medicaid Recipients with Vital Social Services
A new screening program available to eligible Medicare and Medicaid patients of Waianae Coast Comprehensive Health Center, Kalihi-Palama Health Center and The Queen’s Medical Centers aims to address critical gaps between clinical care and social services.
UnitedHealthcare and Optum Take Action to Support People Affected by Severe Weather in Texas
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people affected by severe weather across parts of Texas.
UnitedHealthcare and Optum Take Action to Support People Affected by Severe Weather in Mississippi
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people affected by severe weather across parts of Mississippi.
UnitedHealth Group Reports First Quarter 2019 Results
Strong, well-diversified performance continued across UnitedHealth Group (NYSE: UNH) in first quarter 2019.
UnitedHealthcare and Optum Take Action to Support People Affected by Flooding in Louisiana
UnitedHealthcare and Optum, the health benefits and services companies of UnitedHealth Group (NYSE: UNH), are taking action to help people affected by recent flooding across parts of Louisiana.
UnitedHealthcare Expands Use of Bundled Payments with Medicare Advantage Health Care Providers
UnitedHealthcare is advancing its collaboration with care providers and the government to deliver high-quality care and help people live healthier lives with the UnitedHealthcare Care Bundles Program.

United Health Foundation Partners with Lighthouse Youth & Family Services to Expand Behavioral and Physical Health Services
An $840,000 grant from the United Health Foundation will enable Lighthouse Youth & Family Services to expand access to behavioral and physical health services for more than 5,000 transitioning and homeless children and young adults in the Cincinnati area over the next three years.
UnitedHealthcare to Continue Serving Arizonans Statewide Through the Department of Economic Security Division of Developmental Disabilities Health Plan
The Arizona Department of Economic Security (DES) Division of Developmental Disabilities (DDD) has selected UnitedHealthcare Community Plan of Arizona as one of the contractors to administer the DDD Health Plan for its members effective Oct. 1, 2019.
UnitedHealthcare and the AMA Collaborate to Understand and Address Social Barriers Preventing People’s Access to Better Health
UnitedHealthcare and the American Medical Association announced a new collaboration that will better identify and address social determinants of health to improve access to care and patient outcomes.
Statements
UnitedHealth Group Announces Executive Leadership Team Changes
UnitedHealth Group announced leadership changes consistent with its longstanding, intentional approach to developing an executive team with a range of experiences across its diverse portfolio of businesses and in ongoing service to its mission and the people it serves.
Statement Regarding Medicare Advantage
Update on Texas Hospital Matter
UnitedHealth Group’s Response to the Wall Street Journal’s Recent Reporting on Medicare Advantage
UnitedHealth Group Responds to Misinformation
UnitedHealth Group today issued the following update.
UnitedHealth Group Provides Fact Sheet on Medical Claims
UnitedHealth Group today provided the following information regarding UnitedHealthcare’s medical claims approval rate.
UnitedHealth Group Statement on Today’s Events
We are deeply saddened and shocked at the passing of our dear friend and colleague Brian Thompson, the CEO of UnitedHealthcare.
Optum responds to Department of Justice lawsuit
Following the DOJ legal action aimed at blocking the proposed combination of Optum and Amedisys, Optum has issued the following statement.
Optum Rx Responds to FTC Action
PBMs, like Optum Rx, are the key counterweight to pharmaceutical companies’ otherwise unchecked monopoly power to set and raise drug prices.
UnitedHealth Group’s Response to the Wall Street Journal
Setting the record straight on HouseCalls, Medicare Advantage and the demonstrably superior health outcomes and cost savings delivered to more than 33 million American seniors each year.
Articles
America’s Health Rankings report highlights gains, challenges in women and children’s health
Securing homes for our veterans
Optum Rx increases reimbursement on brand drugs for 2,300 community and independent pharmacies
The future of care: Ambulatory Surgery Centers deliver faster care, lower costs and better outcomes
How the Rapid Treatment Clinic personalizes post-surgery care
The Rapid Treatment Clinic is a popular resource for anyone who needs care and doesn’t need to be in the emergency room. Patients appreciate the convenience, lower out-of-pocket costs and the ability to receive high-quality treatment while minimizing disruptions to their daily lives. The Rapid Treatment Clinic saves them time and provides them with the care they need.
Optum Rx removes reauthorization requirements for an additional 60-plus drugs
Effective July 1, Optum Rx will eliminate reauthorization requirements for an additional 60-plus drugs treating chronic conditions, improving access for patients.
How clinical decision support tools can help redefine patient care
In a recently published article, Dr. McKinley Glover IV, vice president of clinical decision support at Optum Insight, shares the importance of technology to the shift toward value-based care.
UnitedHealth Group’s affordable housing investments surpass $1.2B
UnitedHealth Group has now invested more than $1.2 billion in affordable housing and mixed-income housing developments since 2011, continuing its commitment to address social drivers of health.
Home delivery of prescription drugs improves access and produces savings
Health care is changing to keep up with what people need and want. Here’s how Optum® Home Delivery Pharmacy offers convenience and saves money for patients.
Study: Medicare Advantage enrollees see superior health outcomes under fully accountable care models
A new peer-reviewed paper published in the American Journal of Managed Care shows Medicare Advantage enrollees whose physicians were under fully accountable models have dramatically better health outcomes than patients enrolled in traditional fee-for-service Medicare, even when cared for by the same physicians.
Achieving superior patient outcomes through personalized patient care and clinical excellence
With dedication, expertise and compassion at the forefront of everything they do, Optum Infusion’s 800+ nurses make a profound impact on the lives of those they serve.
America’s Health Rankings® 2025 Senior Report reveals improvements and challenges for older adults
The America’s Health Rankings® 2025 Senior Report examines 55 measures of health, drawn from 24 distinct data sources to present a comprehensive overview of the health and well-being of the nation’s older adults in each of the 50 states and Washington, D.C.
United Health Foundation partners with Cherokee Health Systems to improve access to health care in rural areas
As part of our commitment to improve health outcomes, the United Health Foundation has partnered with Cherokee Health Systems to expand and enhance a prescription delivery program.
United Health Foundation announces $7 million in grants to improve maternal and infant health outcomes
The United Health Foundation announced more than $7 million in new grant partnerships to increase access to maternal and infant health care, address gaps in care for women and children, and to grow and support the doula workforce in Georgia, Michigan, New Mexico and Wisconsin.
Providing a differentiated pharmacy experience through patient-centered care
At Genoa Healthcare and PharmScript, part of Optum Rx, pharmacists are a critical part of the care team who work hand-in-hand with providers to deliver high-quality, convenient patient-centered care.
Exploring the spillover effects of Medicare Advantage risk payment arrangements
In a new peer-reviewed paper published in the American Journal of Managed Care, findings show traditional Medicare patients cared for by physician groups operating under accountable, value-based care arrangements with Medicare Advantage (MA) plans have better health outcomes.
Optum Rx partnership with TennCare provides diapers in first-of-its-kind pharmacy benefit
As part of a recent partnership to support a healthy environment for growth and development for children in Tennessee, Optum Rx teamed with TennCare, Tennessee’s Medicaid program, to provide free diapers for Tennessee children through the pharmacy benefit.
Clinically led services, support and access to medications help those with rare conditions
Optum Frontier Therapies is specifically designed to support the evolution of a rare disease patient’s needs and provide care throughout their journey with monitoring of progress and symptoms, and partnerships with providers, to help achieve optimal therapeutic outcomes.
Florida A&M Optum Rx partnership focused on culturally relevant care
Students benefiting from the first year of Optum Rx’s scholarship program with Florida Agricultural and Mechanical University (FAMU) – a historically Black university in Tallahassee, Florida – say the program has enabled them to prioritize their work inside the classroom to help prepare for careers in pharmacy.
Optum Health primary care practices outperform competitors when treating Medicare Advantage patients
Medicare Advantage patients visiting an Optum Health primary care practice with employed physicians receive better care at a lower total cost than those who visit hospital-based and physician-owned practices, according to new research from UnitedHealth Group.

Medicare Advantage value-based care demonstrates superior patient outcomes
Medicare Advantage beneficiaries in value-based MA plans where doctors are accountable for the cost and quality of care experience better outcomes, according to peer-reviewed research.
Value-based care: Putting the patient first
Value-based care is a UnitedHealth Group ambition grounded in our ability to create connections across care delivery, technology, pharmacy, benefits and financial services – centered around the patient and provider.
In-home care: Meeting patients where they are
Today, nearly half of the 13 million people who are dually eligible for Medicare and Medicaid are not in good health. The home is becoming an optimal setting for delivering value-based care, especially for patients who are most in need and have limited access to care.
Surest: The evolution of health benefits
When UnitedHealth Group set out to reimagine consumer benefits two years ago, we asked consumers what they wanted from a health plan now and in the future. Three out of four wished their health care experiences were more personalized, citing cost savings as the most critical factor.
Optum innovation can reduce median out-of-pocket costs to just $5 for specialty patients, helping to make medications more affordable and accessible
Optum Savings IQ™ enables automation of search and enrollment in financial assistance programs from all sources and helps to save patients more than $2,500 annually.
Tech advances improve risk assessment and breast cancer management
As we observe Breast Cancer Awareness Month, clinicians should be cognizant of ways technology is enhancing our ability to assess patients’ risk of developing breast cancer, and to drive appropriate diagnostic testing and treatment earlier.
Optum Rx deepens support for independent pharmacies with a focus on better health outcomes, enhanced access in rural areas
Today, millions of Americans live miles away from access to their essential medications, while skyrocketing drug prices, set by manufacturers, are squeezing reimbursement pharmacists receive when dispensing a drug. Low-income communities disproportionately lack access to pharmacies due to transportation barriers, systemic inequalities and distance. As a result, individuals in these communities have a harder time adhering to medication schedules and experience wider health disparities.
Optum Rx automates prior authorization process for prescription drugs to improve the patient and provider experience
Optum Rx PreCheck Prior Authorization reduces physician administrative burden and expedites prior authorization approvals
New America’s Health Rankings data brief highlights maternal and infant health disparities
Healthy women and children are the foundation of communities across the country – and it is critical to understand the disparities they face.
UnitedHealth Group’s Response to the Wall Street Journal
Setting the record straight on HouseCalls, Medicare Advantage and the demonstrably superior health outcomes and cost savings delivered to more than 33 million American seniors each year.
Putting patients at the center of care
Health systems are increasingly moving toward value-based care, a model that prioritizes early intervention, rewards high-quality care, delivers better outcomes and drives lower costs. Caitlin Zulla, Optum Health East CEO, discussed what’s needed for a successful transition to value-based care at the Wharton School of the University of Pennsylvania’s Health Care Business Conference in Philadelphia earlier this year.
Revitalizing affordable, healthy housing in East Point, Georgia
UnitedHealth Group partnered with housing developer the Vecino Group, the National Affordable Housing Trust (NAHT) and the East Point Housing Authority (EPHA) on the $24 million redevelopment of a property that has been closed since 2004 and now includes 88 affordable one- and two-bedroom apartments for families earning between $30,000 and $40,000 annually.
New: America’s Health Rankings 2024 Senior Report reveals progress and ongoing challenges for older adults
The recently released 12th edition of the America’s Health Rankings® 2024 Senior Report provides a comprehensive view of the health of America’s older adults, capturing key trends, successes and challenges across 52 measures of health and well-being.
Optum Rx announces new pricing model to offer clients another transparent, predictable way to manage drug trend
Building upon Cost Made Clear payment solutions announced last year, Optum Rx continues to lead the industry with innovative, varied solutions that support demand for transparency and choice while addressing rising drug trend.
UnitedHealth Group releases 2023 Sustainability Report
UnitedHealth Group, in its newly released 2023 Sustainability Report, details progress in helping people live healthier lives and help make the health system work better for everyone.
UnitedHealth Group’s affordable housing investments surpass $1B
UnitedHealth Group has invested more than $1 billion in affordable housing, a major milestone in its ongoing commitment to advancing health equity.
United Health Foundation partners with Native American Connections to increase health care access
The three-year, $2 million grant partnership will provide integrated behavioral health and primary care for Native Americans and underserved individuals and families living in Phoenix, Arizona.
UnitedHealth Group launches new renewable energy investments to support emissions reduction targets
UnitedHealth Group is advancing a sustainable future through two new renewable energy initiatives: a 15-year virtual power purchase agreement (VPPA) with Ørsted and a separate investment in a renewable solar project owned by Swift Current Energy
Optum Rx community and independent initiatives support patients and pharmacists
Recently launched initiatives by Optum Rx enable more than 26,000 in-network community and independent pharmacies with expanded support to strengthen access to care and improve outcomes for the patients they serve
America’s Health Rankings 2023 annual report: Chronic conditions on the rise
Just released, the America’s Health Rankings 2023 Annual Report shows eight chronic conditions have reached the highest prevalence in the report’s history. These include arthritis, asthma, cancer, cardiovascular diseases (CVDs), chronic kidney disease (CKD), chronic obstructive pulmonary disease (COPD), depression and diabetes.
Partnership with Children’s Minnesota uses data to address flu vaccination disparities
Enabled by a $3 million grant partnership with the United Health Foundation, Children’s Minnesota has taken a data-driven approach to reduce flu vaccination disparities among thousands of underserved kids in the Twin Cities.
United Health Foundation donations to help provide humanitarian relief to civilians in Israel and Gaza
In response to the growing humanitarian crisis, the United Health Foundation, the philanthropic foundation of UnitedHealth Group, is donating $1 million to Save the Children and Direct Relief to help with urgent needs such as food, water and medical supplies in Israel and Gaza.
'Barbershop Bashes' help reduce health disparities through cancer screening
Isiah Skinner Jr., owner of Skinner’s Barbershop in Morgan City, La., has been hosting annual Barbershop Bash events since 2013 as a way for men to receive free, preventive cancer screenings and education.
New America’s Health Rankings report: Rising maternal mortality, mental health challenges among women
This year’s report builds on the America’s Health Rankings platform’s longstanding commitment to better understand the comprehensive health and well-being of women and children by analyzing the latest data on 122 measures from 34 distinct data sources.
Deploying technology to address America’s mental health and clinician burnout crisis
At the recent Aspen Ideas Health event in Colorado, Optum Health Chief Nursing Officer Kristy Duffey shared ways UnitedHealth Group is using technology to increase access to mental health care for patients and reduce workplace stress for clinicians.
Optum Rx scholarship fund helps support underrepresented pharmacy students at Florida A&M University
Representation of minorities among pharmacy professions is lacking, with access to funding for graduate pharmacy programs among the top barriers contributing to low numbers of underrepresented students enrolled in pharmacy schools.
New data brief highlights mental and behavioral health disparities
As communities across the country recover from the health effects of the pandemic, individuals are feeling the impact of mental and behavioral health challenges.
UnitedHealth Group value-based care strategies featured in Fortune
A recent Fortune article provided an in-depth look at value-based care, sharing strategies deployed by UnitedHealth Group and others.
HouseCalls visits associated with fewer emergency visits, hospital stays for Medicare Advantage patients
Medicare Advantage patients who received in-home, preventive wellness assessments via the Optum HouseCalls program spent less time in emergency room and inpatient hospital settings, researchers at Yale Medicine working in collaboration with Optum have found.
Optum Rx introduces new initiatives to improve the pharmacy experience for community and independent pharmacy partners and patients
Solutions are designed to ensure the more than 26,000 community and independent pharmacies in our network can support expanded access to care, improve outcomes for the patients they serve and remain competitive.
Optum Rx launches pharmacy wellness programs to support underserved and rural communities
New, innovative partnerships between Optum Rx and community pharmacies aim to expand access to care, preventive services, and medication adherence and improve health outcomes in underserved communities.
UnitedHealth Group named a top community-minded company
For the 11th consecutive year, Points of Light named UnitedHealth Group one of the 50 most community-minded companies in America based on its annual Civic 50 survey.
New report highlights urgent need to support older Americans post-pandemic
According to the United Health Foundation’s America’s Health Rankings 2023 Senior Report, early death and drug death rates continued to increase.
New Optum Rx payment solutions continue to empower clients with more choice, transparency
New offerings build on our history of bringing innovation to employers, unions, health plans and consumers to help improve affordability and transparency in pharmacy benefits.
Partnering to provide access to care for children in Arizona
A $3 million United Health Foundation grant to Valle del Sol Community Health helped provide primary and behavioral care for thousands of students from underserved communities around Phoenix.
Partnership aims to improve mental health care for LGBTQ+ and BIPOC youth
A $2M United Health Foundation grant to Rainbow Health will help support the behavioral health and well-being of LGBTQ+ and BIPOC youth in Minnesota
UnitedHealth Group partners with Morehouse School of Medicine to help Black mothers access health care resources
UnitedHealth Group has partnered with Morehouse School of Medicine to introduce a new mobile app that aims to connect new Black mothers living in Georgia’s underserved communities with resources to help sustain their overall health and their child’s well-being.
United Health Foundation working to diversify the health workforce
Ten-year, $100 million commitment is providing scholarships for underrepresented current and future health professionals.
Partnering with East Carolina University to expand youth access to mental health care services
$3.2M United Health Foundation grant will support the mental health and well-being of underserved youth in North Carolina.
Partnering with Children’s Minnesota to reduce disparities and improve access to care
The United Health Foundation and Children’s Minnesota are taking aim at disparities in the Twin Cities around asthma, vaccinations and mental health through a three-year, $3 million grant partnership
Chief Medical Officer Dr. Margaret-Mary Wilson discusses social determinants of health for seniors
During a recent Axios event, Dr. Wilson talked about UnitedHealth Group’s holistic approach to health in Medicare Advantage.
UnitedHealth Group grant helps build more diverse child and adolescent psychiatry workforce
Through the four-year, $4 million grant, announced in 2020, UC San Diego School of Medicine launched the Child and Adolescent Psychiatry Inclusive Excellence Program (CAPIE), an innovative approach to building a more diverse child and adolescent psychiatry (CAP) workforce
Expanding behavioral health services to help individuals experiencing homelessness
The National Health Care for the Homeless Council (NHCHC) will integrate behavioral health services in medical respite programs across three states thanks to a three-year, $2.9 million grant awarded by the United Health Foundation
Mortality measures during COVID-19 continue to reflect deep racial disparities according to America’s Health Rankings 2022 Annual Report
Report features key findings from the COVID-19 era, including increases in premature death and drug deaths

United Health Foundation partnership aims to decrease nurse burnout and attrition
The United Health Foundation has announced a three-year, $3.1 million grant partnership with the American Nurses Foundation to reduce burnout with an emphasis on nurses of color and those under age 35 through implementation of the Building Blocks for Beating Burnout (B4) program.
UnitedHealth Group honors apprenticeship cohort graduates
Program aims to improve equity by diversifying our workforce to reflect the communities we serve
America’s Health Rankings reveals continued youth mental health crisis
Three-year grant partnership with Active Minds will address increases in youth mental health challenges revealed by the 2022 America’s Health Rankings Health of Women and Children Report.
Improving prescription drug affordability with $0 copays
“High prices are a significant barrier to prescription drugs for many people, so we are using our unique capabilities to deliver savings for consumers,” said Brian Thompson, chief executive officer of UnitedHealthcare.
Clinician harnesses technology to improve care and increase efficiency
While participating in the Center for Clinician Advancement's Clinician Leader Executive program, Nimita Varga, clinical services manager, Optum Hospice Pharmacy Services, discovered a way to potentially improve care and increase efficiency.
National Physicians Week spotlight: Leading change for improved physician well-being
Discover how a physician wellness training program offered by the American Academy of Family Physicians in partnership with the United Health Foundation helped two participants improve their well-being and reduce burnout in their organizations.
Partnership with HealthNet expands access to care
The United Health Foundation has launched a partnership with HealthNet, a nonprofit health care provider serving Indiana, to expand access to primary and behavioral health care in Morgan and Monroe counties in Indiana, as well as low-income areas in Indianapolis.
Break the bias: Celebrating International Women’s Day
UnitedHealth Group joins the world in celebrating International Women’s Day and its #BreakTheBias theme for 2022.
New Research Examines Benefits of High-Performing Skilled Nursing Facilities
High-performing skilled nursing facilities could prevent 100,000 Medicare hospital readmissions per year and save $56 billion over 10 years, according to new UnitedHealth Group research.
Black History Month spotlight: Leye Oyetunji models, spreads joy among clinicians
Learn how Leye Oyetunji models and spreads joy to support his team of pharmacy care specialists at a time many clinicians are experiencing burnout during the COVID-19 pandemic.
Celebrating Black History Month
Throughout February — and every day — we reflect, recognize and appreciate Black Americans’ role in shaping the success of our nation, our company and those we serve.
Optum launches new Evidence Engine to advance genomics-based disease detection and treatment
Optum Evidence Engine’s first project in partnership with Illumina.
Addressing Critical Health and Wellness Needs in the San Francisco Bay Area
Optum and John Muir Health are building on first-year results of a $1 million three-year pro bono collaboration launched in 2020 to address critical health and wellness needs in the San Francisco Bay Area.
New Report Reveals a Complex Picture of Americans’ Health
The picture of Americans’ health and well-being during the early stages of the COVID-19 pandemic is complex and nuanced, according to the UnitedHealth Foundation’s 2021 America’s Health Rankings Annual Report.
UnitedHealth Group Strengthens Its Commitment to Environmental Health
Today at our annual Investor Conference, CEO Andrew Witty spoke about the importance of sustainability and made two announcements aimed at strengthening our commitment to environmental health and minimizing our impact on climate change.
Building Bioinformatics Program for Students at Historically Black University
The United Health Foundation is collaborating with Harris-Stowe State University to help address the gap in the number of diverse college students trained in biomedical sciences.
Virtual Event Features Our Efforts to Address Health Disparities for Children and Families
During a recent Washington Post Live virtual panel discussion, Dr. Margaret-Mary Wilson, executive vice president and associate chief medical officer, UnitedHealth Group, talked about key drivers to improving health outcomes within underserved communities.
Working Toward a Future Where Health Care is Simple, Efficient and Easy to Navigate
Improving the experience for the people we serve.
Honoring the Passion and Perspectives of Our Veteran Colleagues
Veterans are a valuable and integral part of UnitedHealth Group, and during a recent panel discussion we solicited their thoughts on wellness, resiliency and success.
Helping Children Access Care in Our Nation’s Capital
A three-year, $3.4 million United Health Foundation grant to Children’s National Hospital will help expand access to health care for school-aged children in underserved communities in Washington, D.C.
UnitedHealth Group Supports Removing Race From Key Kidney Care Diagnostic Equation
A National Kidney Foundation and American Society of Nephrology recommendation to eliminate race from a key diagnostic equation aligns with UnitedHealth Group’s commitment to remove race from clinical decision algorithms, care delivery and research.
Enhancing the Delivery of Mental Health Care
UnitedHealth Group is working to address the growing need for mental health services with a variety of virtual platforms and in-person offerings that provide more convenient access to high-quality care and result in improved health outcomes.
New Health Report Identifies Need to Address Mental and Behavioral Health Among Teens and Children in the U.S.
Anxiety among children and teen suicide increased significantly before and during the pandemic, underscoring the urgent need for a continued focus on behavioral health support.
Expanding Access to Convenient, High-Quality Health Care in the Home
Compassionate, clinician-led solutions create “golden opportunities”.
Redefining Mental Health Care With Peer Support
Niquita Ervine, Peer Support Specialist, strengthens the consumer experience through advocacy.
Joy Fitzgerald, UnitedHealth Group’s Chief Diversity, Equity and Inclusion Officer, Shares Her Passion for a Brighter Future
Celebrating boldness and authenticity on Women’s Equality Day and every day.
Our Commitment to Sustainability: In the Words of Dr. Margaret-Mary Wilson
Executive Vice President and Chief Medical Officer of UnitedHealth Group, Dr. Margaret-Mary Wilson, discusses how we’re creating a sustainable health care system.
Partnership Aims to Expand Access to Behavioral Health Care in Washington State
Nationwide, behavioral and mental health challenges are rising and have been exacerbated by COVID-19. In Washington state, the mental and behavioral health needs of children and adults are an increasing concern.
Empowering Health Grants Help Expand Access to Care
UnitedHealthcare is awarding $11.4 million in Empowering Health grants across 18 states and the District of Columbia to help address these needs for uninsured individuals and underserved communities.
New America’s Health Rankings Report Reveals Urgent Need to Address Health Disparities
Widespread health disparities persisted across racial, ethnic, gender, geographic and educational lines before the COVID-19 pandemic, according to the United Health Foundation’s inaugural America’s Health Rankings Health Disparities Report.
Pride Month Celebrates an Ongoing Effort to Educate and Reflect
This month, Optum (part of UnitedHealth Group) launched two initiatives to help advance LGBTQ+ health equity and cultural competency within and outside the organization.
Points of Light Names UnitedHealth Group Top Community-Minded Company
UnitedHealth Group has been named to The Civic 50 for the 10th consecutive year and honored for the fourth time as the sector leader for health care since the survey began in 2012.
New Partnership Expands Access to Prenatal Care
The United Health Foundation has committed $3 million to CAMBA, Inc. to improve access to prenatal care for underserved and homeless women in New York City.
Helping 11,000 Children Access Care
A $3 million grant to Valle del Sol Community Health, a federally qualified health center in the greater Phoenix area, will support the purchase of three mobile medical units and fund three mobile care teams to reach thousands of young people with coordinated primary and behavioral health care.
New Report Identifies Growing Challenges for Older Americans
Even prior to the COVID-19 pandemic, U.S. seniors were facing increased mental health challenges including increased drug deaths, suicide and frequent mental distress, according to a new report released today by America’s Health Rankings®.
Partnership Aims to Help Businesses Following Civil Unrest
UnitedHealth Group provided a $500,000 grant to the Neighbors United Funding Collaborative to help St. Paul, Minnesota businesses — such as Lloyd’s Pharmacy in the Hamline-Midway neighborhood — reopen, rebuild and in some cases relocate following civil unrest last summer.
Mobile Health Teams Provide Health Care Access Amid Pandemic and Following Civil Unrest
A $1 million grant to Minnesota Community Care supports the use of mobile health teams and school-based clinics to serve underserved youth in St. Paul with primary care, mental health support, social work services and pharmacy services during the pandemic, among several other programs.
Chief Medical Officer of Maternal-Child Health Discusses Addressing Health Disparities in Maternal Care
The mortality rate for expectant Black mothers in America is twice as high as white mothers, according to America’s Health Rankings data. This is one of the widest disparities in women’s health, according to the report, but there are many more.
United Health Foundation Support Fuels Medical School Charter Graduation
The United Health Foundation is working to address primary care physician shortages in Nevada while helping improve residents’ overall health and access to care.
Expanding Access to Maternal Health Care in Nevada
The United Health Foundation is working to improve access to prenatal care in underserved communities in Nevada and help grow the state’s OB-GYN and family medicine physician workforce.
New Collaboration Targets Urgent Health Challenges in Colorado
UnitedHealth Group’s Rocky Mountain Health Plans has announced a $30 million commitment to address important health issues in Colorado.